Wolff-Parkinson-White (WPW) — ECG Rhythm | Telemetric Pro
A pre-excitation syndrome where an accessory pathway (bundle of Kent) bypasses the AV node, producing the classic triad: short PR interval, delta wave (slurred QRS upstroke), and widened QRS complex.
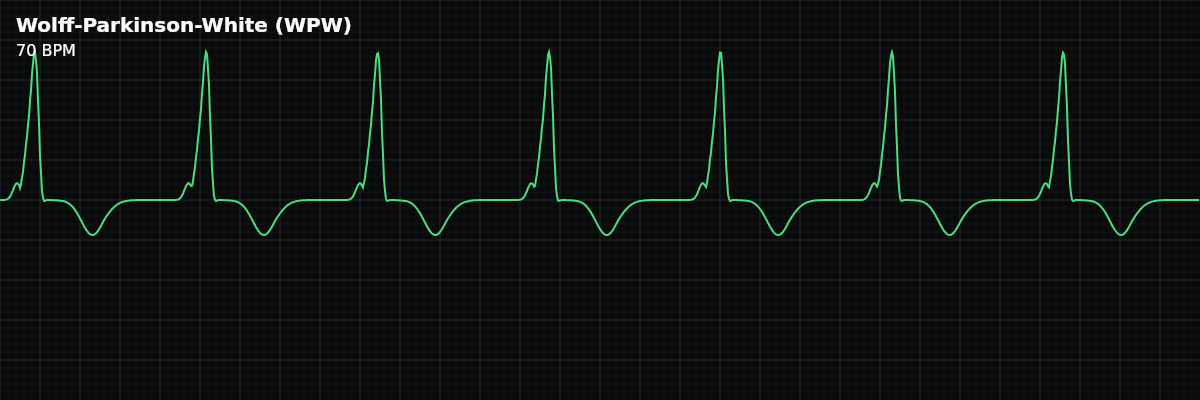
| Rate | Any (pattern present at baseline) |
|---|---|
| Rhythm | Regular (at baseline) |
| P Waves | Normal (SA node fires normally) |
| PR Interval | < 0.12 s (short) |
| QRS Duration | > 0.11 s (widened by delta wave) |
Wolff-Parkinson-White is a congenital condition where an extra electrical pathway — the bundle of Kent — connects the atria directly to the ventricles, bypassing the normal AV nodal delay. At baseline, this produces a distinctive ECG pattern: the impulse reaches the ventricles early (short PR), begins depolarizing the ventricular muscle slowly (delta wave), and then the normal His-Purkinje system catches up (the rest of the QRS).
For monitor technicians, WPW matters because it creates the potential for life-threatening tachyarrhythmias. The accessory pathway can participate in re-entrant circuits (causing AVRT) or can rapidly conduct atrial fibrillation directly to the ventricles at dangerously fast rates. Recognizing the WPW pattern on a baseline ECG alerts the team to this risk.
What Changed from Normal Sinus Rhythm
WPW changes three things from NSR: the PR interval (shortened because the impulse bypasses the AV node), the beginning of the QRS (slurred delta wave from early muscle-to-muscle conduction), and the QRS width (widened by the delta wave). The P waves are normal — the SA node fires on schedule. The overall rhythm is regular. Everything looks like NSR except for the characteristic pre-excitation pattern.
Five Criteria: WPW vs NSR
- Rate: Any (baseline pattern, not rate-dependent)
- The WPW pattern is present at any heart rate. It is a fixed anatomic pathway, not a rate-related phenomenon. The pattern may be more or less obvious at different rates.
- Regularity: Regular (at baseline)
- The baseline rhythm is regular sinus with the pre-excitation pattern. Tachyarrhythmias (AVRT, AFib) are complications, not the baseline pattern.
- P Waves: Normal (the SA node fires normally)
- P waves are upright and normal. The pre-excitation only affects how the impulse reaches the ventricles — atrial depolarization is unaffected.
- PR Interval: Short (<120ms)
- Shortened because the impulse bypasses the AV nodal delay via the accessory pathway. This is the "pre" in pre-excitation — the ventricles are activated earlier than normal.
- QRS: Widened (>110ms) with delta wave
- The QRS begins with a slurred upstroke (delta wave, 30-50ms) representing early muscle-to-muscle conduction, then sharpens as the His-Purkinje system takes over. Total QRS is typically 110-160ms.
What WPW Looks Like on the Strip
On the strip, WPW has a distinctive look: the PR interval is unusually short, and the QRS begins with a gentle, slurred slope (the delta wave) rather than the sharp, crisp onset of a normal QRS. The QRS is wider than normal because the delta wave adds extra time to the beginning. Once you learn to spot the combination of short PR + delta wave, WPW is recognizable at a glance.
The Dangerous Scenario: AFib with WPW
The most dangerous situation in WPW is atrial fibrillation. In normal AFib, the AV node acts as a gatekeeper — it limits how many impulses reach the ventricles (typically 120-180 BPM). But in WPW with AFib, the accessory pathway has no such rate-limiting function. It can conduct the chaotic atrial impulses directly to the ventricles at rates exceeding 250 BPM — fast enough to degenerate into ventricular fibrillation.
Going Deeper — AVRT Types in WPW
The accessory pathway creates two distinct reentrant tachycardia circuits — understanding both helps you interpret what you see on the monitor when a WPW patient develops a tachyarrhythmia:
Clinical Context for Monitor Technicians
WPW affects approximately 1-3 per 1000 people. Many are asymptomatic and the pattern is found incidentally. The distinction between WPW pattern (ECG finding only) and WPW syndrome (pattern + symptomatic tachyarrhythmias) is important clinically. The delta wave may be subtle or intermittent — it can come and go, and may be visible in some leads but not others.
Going Deeper: WPW — The "Great Mimic"
When to Escalate
**Notify immediately:** - New WPW pattern (first documentation — needs evaluation) - Any tachyarrhythmia in a patient with known WPW - Irregular wide-complex tachycardia in a WPW patient (possible AFib with pre-excitation — most dangerous) - Patient symptomatic with palpitations, near-syncope, or syncope **Document and monitor:** - Known, stable WPW pattern at baseline without symptoms - Intermittent pre-excitation (delta wave comes and goes)
Medication Safety — Why It Matters on the Monitor
AV nodal blockers — adenosine, diltiazem, verapamil, digoxin, and beta-blockers — are dangerous in WPW with atrial fibrillation. The mechanism is straightforward: blocking the AV node removes the only rate-limiting pathway. All conduction is forced through the accessory pathway, which has no built-in speed limit. The accessory pathway can conduct at 300+ bpm, and at those rates the ventricles cannot recover between beats. The result is degeneration into ventricular fibrillation.