Asystole — ECG Rhythm | Telemetric Pro
The absence of all electrical activity in the heart. This is cardiac arrest — the heart has stopped generating any organized impulses.
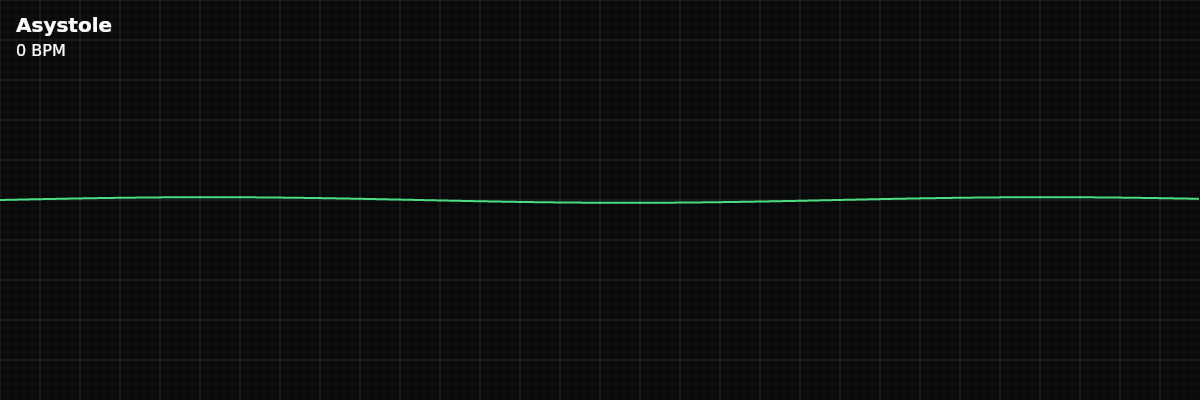
| Rate | 0 bpm (no electrical activity) |
|---|---|
| Rhythm | Flatline |
| P Waves | Absent |
| PR Interval | Not applicable |
| QRS Duration | No QRS complexes |
Asystole is the end of the line. In VFib, the heart is at least trying to do something — the electrical activity is chaotic, but it exists, and defibrillation can reset it. In asystole, even that chaotic activity has stopped. The heart has ceased generating any electrical impulses at all. The monitor shows a flatline.
For monitor technicians, asystole presents a unique challenge: it looks exactly like a disconnected lead. A flatline on the monitor could mean the patient is in cardiac arrest, or it could mean an electrode fell off. The difference between these two possibilities could not be more consequential, which is why confirming asystole — not just seeing it — is a critical skill.
What Changed from Normal Sinus Rhythm
Asystole is not a deviation from NSR — it is the absence of all electrical activity. Every waveform, every interval, every measurable feature of the ECG is gone. The five-criteria method cannot even be applied because there is nothing to evaluate.
What Asystole Looks Like on the Strip
The tracing is essentially a flat line. There may be minor baseline drift from electrical noise or electrode contact, but there are no P waves, no QRS complexes, no T waves, and no fibrillatory oscillations. The monitor may display a heart rate of zero or show dashes where the rate would normally appear.
Confirming Asystole: The Three Checks
Before treating a flatline as real asystole, three checks must be performed. These exist because a flatline has multiple possible causes — only one of which is cardiac arrest.
**1. Check Multiple Leads** — Low-amplitude VFib can appear as a flatline in one lead but show visible fibrillatory activity in another. Switch leads and verify the flatline persists in at least two different views. **2. Check Lead Connections** — A disconnected electrode produces a perfect flatline. During patient movement or code situations, electrodes commonly fall off. Physically verify all electrodes are attached to the patient's skin and cables are plugged into the monitor. **3. Increase Gain** — Very low-amplitude VFib may not be visible at standard gain settings. Turn the monitor gain to maximum. If chaotic fibrillatory waves appear, the rhythm is VFib (shockable) — not asystole.
Asystole vs Low-Amplitude VFib
This is the most critical distinction in cardiac arrest rhythm recognition. Both can appear as near-flatlines on the monitor, but the treatment is completely different: **Asystole** — True flatline with no electrical activity. NOT shockable. Treatment is CPR and medications. **Low-amplitude VFib** — Chaotic oscillations that may look almost flat but show fibrillatory activity when you check a second lead or increase gain. IS shockable. Defibrillation can terminate the rhythm and allow the heart to restart. When you are unsure, the safest approach is to assume VFib and let the code team make the determination. The two-lead confirmation and gain check exist precisely for this situation.
Clinical Context for Monitor Technicians
Asystole typically represents the end stage of a deteriorating cardiac situation. It may follow VFib that was not treated, or it may develop from progressive bradycardia that slows to a stop. In hospitalized patients, asystole may occur after prolonged illness, massive heart attack, or as a terminal event. It carries the worst prognosis of all cardiac arrest rhythms.