Atrial Paced Rhythm (AAI) — ECG Rhythm | Telemetric Pro
A pacemaker stimulates the atrium, and the impulse conducts normally through the AV node to produce a narrow QRS. Used when the SA node is dysfunctional but AV conduction is intact.
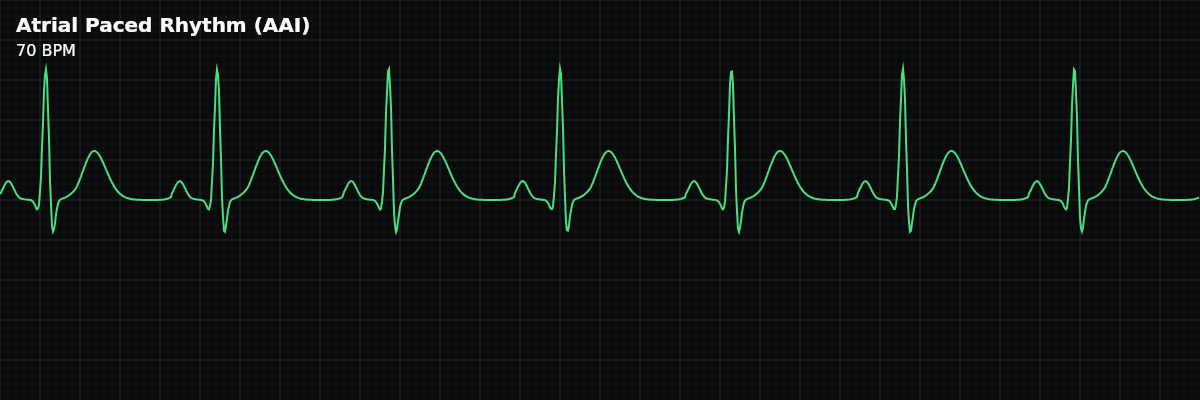
| Rate | 60–70 bpm (programmed) |
|---|---|
| Rhythm | Regular |
| P Waves | Pacing spike before each P wave |
| PR Interval | 0.12–0.20 s (native AV conduction) |
| QRS Duration | < 0.12 s (native QRS) |
Atrial pacing is the simplest form of permanent pacing. The pacemaker replaces the SA node as the atrial pacemaker, but everything else — AV conduction, ventricular depolarization — proceeds normally. This is why the QRS is narrow: the impulse travels from the paced atrium through the AV node and His-Purkinje system exactly as it would in normal sinus rhythm.
For monitor technicians, atrial pacing is the easiest paced rhythm to identify: a spike before the P wave and a normal narrow QRS. The critical monitoring skill is recognizing when atrial pacing fails — if spikes appear without P waves (failure to capture) or if P waves appear without preceding spikes when the rate drops (failure to sense).
What Changed from Normal Sinus Rhythm
Atrial pacing changes one thing from NSR: the source of atrial depolarization. Instead of the SA node initiating the P wave, the pacemaker electrode does. The P wave morphology may look different (because depolarization starts at the pacing electrode, not the SA node), but the PR interval, QRS, and overall rhythm are normal. The narrow QRS confirms that AV conduction is intact.
Five Criteria: Atrial Paced vs NSR
- Rate: Set by pacemaker (typically 60-70 BPM)
- The pacemaker fires at the programmed lower rate limit when the native sinus rate drops below it. If the native rate is faster, the pacemaker inhibits and you see native sinus beats.
- Regularity: Regular
- Paced rhythm is regular at the programmed rate. You may see occasional native sinus beats interspersed if the native rate transiently exceeds the paced rate.
- P Waves: Paced (spike before P wave)
- A sharp pacing spike appears immediately before each P wave. The P wave morphology may differ from sinus because depolarization starts at the electrode, not the SA node.
- PR Interval: Normal (AV conduction intact)
- The impulse travels from the paced atrium through the AV node normally. The PR interval is similar to what you would see in NSR — confirming intact AV conduction.
- QRS Complex: Narrow (<0.12s)
- The ventricles depolarize normally through the His-Purkinje system. A narrow QRS is the hallmark of atrial-only pacing — it confirms that no ventricular pacing is occurring.
What Atrial Pacing Looks Like on the Strip
On the monitor, atrial pacing looks almost like NSR — regular rhythm, narrow QRS, normal rate. The giveaway is the sharp spike immediately before each P wave. If you see spikes before the P waves but NOT before the QRS, you are looking at atrial-only pacing. The narrow QRS confirms that ventricular conduction is working normally.
AAI vs Other Pacing Modes
Understanding where atrial pacing fits in the pacing spectrum: **AAI (Atrial Paced)** — Spike before P only. Narrow QRS. Requires intact AV conduction. **VVI (Ventricular Paced)** — Spike before QRS only. Wide QRS. No AV synchrony. **DDD (Dual Paced)** — May have spikes before both P and QRS. Wide QRS when ventricular pacing occurs. Maintains AV synchrony. **VDD (Atrial Sensed, Ventricular Paced)** — Native P waves (no atrial spike) with spike before QRS. Wide QRS. AV synchrony via sensed P waves.
Clinical Context for Monitor Technicians
Atrial pacing (AAI) is used for sinus node dysfunction (sick sinus syndrome, symptomatic sinus bradycardia) when AV conduction is intact. It preserves the normal ventricular activation sequence, which is hemodynamically superior to ventricular pacing. In practice, pure AAI pacing is becoming less common because most patients receive dual-chamber (DDD) pacemakers as a safety net against future AV block.
When to Escalate
**Notify promptly:** - Spikes without P waves (failure to capture) - Native P waves without preceding spikes when rate drops (failure to sense) - New PR prolongation or dropped beats (developing AV block in an atrial-paced patient) - Patient becomes symptomatic — dizziness, syncope, fatigue **Document and monitor:** - Stable atrial pacing with consistent capture and normal AV conduction - Occasional native beats interspersed (normal behavior when native rate exceeds paced rate)
What Happens When...
**Patient exercises** — In rate-responsive mode (AAIR), the pacemaker detects activity via an accelerometer or minute ventilation sensor and increases the atrial pacing rate. On the monitor, you will see the paced rate climb gradually during activity and return to the programmed lower rate limit at rest. The narrow QRS remains unchanged because AV conduction is still normal — only the atrial pacing rate changes. This is expected behavior, not a malfunction.