Sinus Bradycardia (SB) — ECG Rhythm | Telemetric Pro
A sinus rhythm with a rate below 60 bpm. The SA node fires slower than normal, but every other part of the conduction system works exactly as it should.
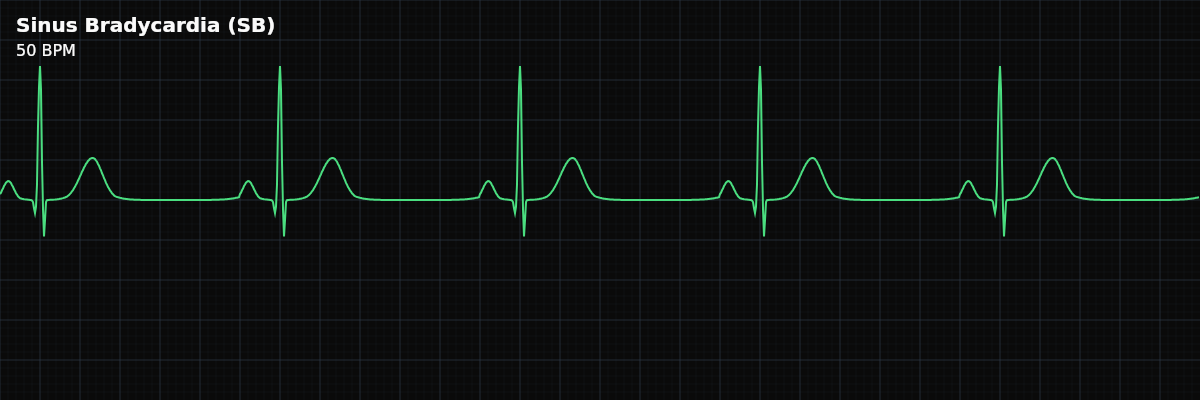
| Rate | < 60 bpm |
|---|---|
| Rhythm | Regular |
| P Waves | Upright, uniform, one before every QRS |
| PR Interval | 120–200 ms (0.12–0.20 sec) |
| QRS Duration | < 120 ms (narrow) |
Why This Rhythm Matters
Sinus Bradycardia is your first example of a *single-criterion deviation* from Normal Sinus Rhythm. Everything about the conduction pathway is intact — same origin, same route, same waveform morphology. The only thing that changed is the speed. Learning to see that distinction is the core skill of rhythm interpretation: identify *what* deviated and *how much* of the system is still working normally.
What Changed: The SA Node Slowed Down
The SA node's firing rate is not fixed — it's continuously adjusted by the autonomic nervous system. Increased parasympathetic (vagal) tone or decreased sympathetic drive slows the SA node below its normal 60–100 bpm range. The impulse still originates in the SA node, still travels through the atria, pauses at the AV node, and conducts through the His-Purkinje system exactly as it does in NSR. The tracing looks the same — the complexes are just spaced further apart.
The Five Criteria: SB vs. NSR
Run the same five-criteria checklist you learned in NSR. Four of the five answers are identical — only the rate has changed.
- Rate: Less than 60 bpm
- RR interval exceeds 1000 ms (25 mm / 5 large boxes). This is the only criterion that differs from NSR.
- Regularity: Regular
- RR intervals are equal throughout. The SA node fires at a constant (slower) rate.
- P waves: Upright, uniform, one before every QRS
- Identical to NSR. Confirms the impulse still originates from the SA node.
- PR interval: 120–200 ms, constant
- Identical to NSR. AV conduction time is unaffected by the slower rate.
- QRS complex: Narrow (< 120 ms), one after every P wave
- Identical to NSR. His-Purkinje conduction is intact.
Rate
The defining feature: a heart rate below 60 bpm, meaning the RR interval exceeds 1000 ms (5 large boxes). The slower the rate, the wider the gap between complexes.
**Rate-to-interval reference:** - **59 bpm** → RR = 1017 ms (just over 5 large boxes) — the boundary - **50 bpm** → RR = 1200 ms (6 large boxes) - **40 bpm** → RR = 1500 ms (7.5 large boxes) - **30 bpm** → RR = 2000 ms (10 large boxes)
Regularity
Sinus Bradycardia is regular — the RR intervals are consistent throughout, just as in NSR. The SA node is still pacing steadily; it's simply pacing more slowly.
P Waves, PR Interval & QRS Complex
These three components are unchanged from NSR — and that's exactly the point. The presence of normal, upright P waves before every narrow QRS with a constant PR interval confirms that the entire conduction pathway below the SA node is functioning normally. The *only* thing different is how often the SA node fires.
If any of these change — inverted P waves, prolonged PR, wide QRS, or missing QRS complexes — the rhythm is no longer simple Sinus Bradycardia. Those findings point to a conduction problem beyond just a slow SA node.
T Waves
T waves in Sinus Bradycardia follow the same rules as NSR: upright, present after every QRS, amplitude below 5 mm. At slower rates, T waves may appear slightly more prominent because there's more baseline between complexes — but the morphology itself hasn't changed.
Clinical Context: Not Always a Problem
A slow rate on the monitor does not automatically mean something is wrong. The same rate of 45 bpm can be completely normal in one patient and concerning in another. What matters is *why* it's slow and *how the patient is doing*.
**Common reasons you'll see it:** - **Athletes** — trained endurance athletes often rest at 40–50 bpm due to enhanced stroke volume - **Sleep** — parasympathetic tone increases naturally during sleep, slowing the rate - **Medications** — beta-blockers, calcium channel blockers, and digoxin commonly slow the SA node - **Vagal response** — coughing, bearing down, or nausea can trigger a temporary drop in rate