Ventricular Tachycardia (VT) — ECG Rhythm | Telemetric Pro
A life-threatening wide-complex tachycardia originating in the ventricles. Can be monomorphic or polymorphic.
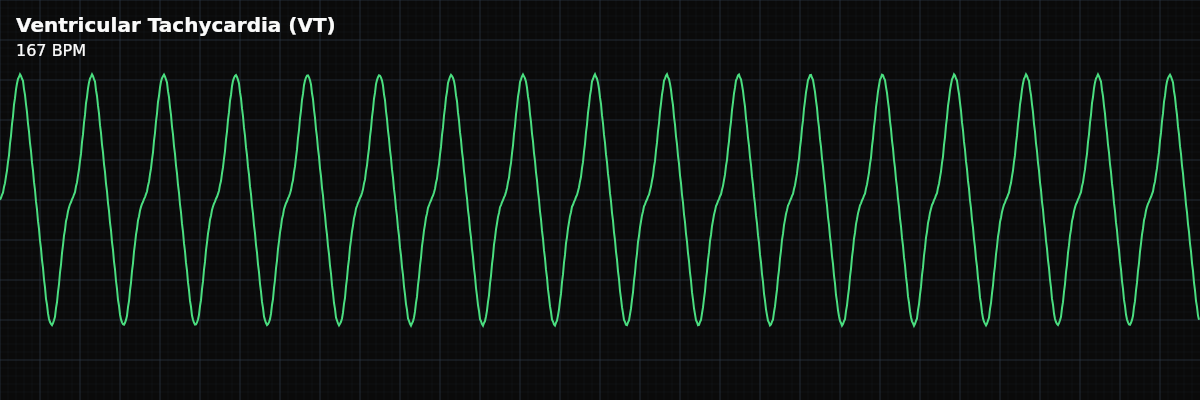
| Rate | 100–250 bpm |
|---|---|
| Rhythm | Regular |
| P Waves | Absent (AV dissociation) |
| PR Interval | Not applicable |
| QRS Duration | > 0.12 s (wide, typically 0.14–0.20 s) |
Every rhythm you have studied so far has been survivable, manageable, and often chronic. Ventricular Tachycardia is different. VT is a life-threatening emergency. A patient in VT can be talking to you one moment and in cardiac arrest the next. The rhythm can deteriorate to Ventricular Fibrillation — a lethal rhythm — without warning.
VT is also the first rhythm where the **wide QRS** is the central identifying feature. In every previous rhythm — NSR, SVT, AFib — the QRS was narrow because the ventricles depolarized through the fast His-Purkinje conduction system. In VT, the impulse originates in the ventricular muscle itself and has to spread slowly through working myocardial tissue. That slow conduction produces a QRS wider than 120ms, often reaching 140-200ms. When you see a wide, fast, regular rhythm on the monitor, VT should be your first thought.
What Changed from Normal Sinus Rhythm
VT changes nearly every criterion from NSR: the rate is dramatically faster, the QRS is wide, P waves are absent or dissociated, and the rhythm is driven by an ectopic ventricular focus rather than the SA node. The only thing that may look similar is the regularity — monomorphic VT is usually regular.
Five Criteria: VT vs Normal Sinus Rhythm
- Rate: 100-250 bpm (NSR: 60-100)
- Most clinical VT runs 150-200 bpm. Slower VT (100-150 bpm) exists and may be briefly tolerated, but any rate of VT is dangerous because the rhythm can accelerate or deteriorate without warning.
- Regularity: Usually regular (same as NSR)
- Monomorphic VT — the most common type — is regular because a single ectopic focus fires at a steady rate. Polymorphic VT, where the QRS morphology varies beat to beat, may be irregular.
- P Waves: Absent or dissociated (NSR: upright, one per QRS)
- The atria continue to fire at their own rate, but these P waves are usually buried inside the wide QRS complexes and invisible. When P waves can be seen marching through at a different rate, this confirms VT.
- PR Interval: Not applicable (NSR: 120-200ms)
- There is no relationship between atrial and ventricular activity, so the PR interval does not exist. The atria and ventricles are electrically disconnected.
- QRS Width: Wide, >120ms (NSR: narrow, <120ms)
- This is the defining feature. VT produces QRS complexes typically 140-200ms wide — that is 3.5 to 5 small boxes on standard paper. The wide, bizarre morphology looks dramatically different from normal QRS complexes.
Rate
VT rates range from 100 to 250 bpm, with most episodes running 150-200 bpm. The rate matters clinically because faster VT is less hemodynamically tolerated — at 200 bpm, the ventricles barely have time to fill before the next contraction, causing blood pressure to drop rapidly.
QRS Complex
The wide QRS is the most important feature of VT. It occurs because the impulse starts in the ventricular muscle and has to spread slowly through tissue rather than traveling the fast His-Purkinje highway. This cell-to-cell conduction takes 140-200ms instead of the normal 80-100ms, producing a wide, bizarre-looking complex that is immediately recognizable.
Monomorphic vs Polymorphic VT
VT comes in two forms, and you need to recognize both on the strip because they look very different.
**Monomorphic VT** — Every QRS complex looks identical because a single ectopic focus fires repeatedly. The rhythm is regular, the morphology is uniform, and the strip has a repetitive, sawtooth appearance. This is the most common type. **Polymorphic VT** — The QRS complexes vary in shape, size, and direction from beat to beat. This indicates either multiple ectopic foci or a shifting reentry circuit. Polymorphic VT is more unstable and more likely to degenerate into Ventricular Fibrillation.
The Critical Rule: Wide = VT Until Proven Otherwise
There are other causes of a wide-complex tachycardia — SVT with aberrant conduction is the most common alternative. But here is the rule that applies to everyone from monitor techs to cardiologists: **approximately 80% of wide-complex tachycardias are VT**. When you see a wide, fast rhythm on the monitor, treat it as VT until someone proves otherwise.
The consequences of getting this wrong are asymmetric. If you call VT and it turns out to be SVT with aberrancy, no harm done — the clinical team will reassess. If you assume SVT when it is actually VT, the patient may receive medications that make the situation worse or lose critical time before definitive treatment.