Second Degree AV Block 2:1 — ECG Rhythm | Telemetric Pro
A fixed 2:1 AV conduction pattern where every other P wave is blocked. Cannot be classified as Type I or Type II from the rhythm alone because no PR pattern is visible.
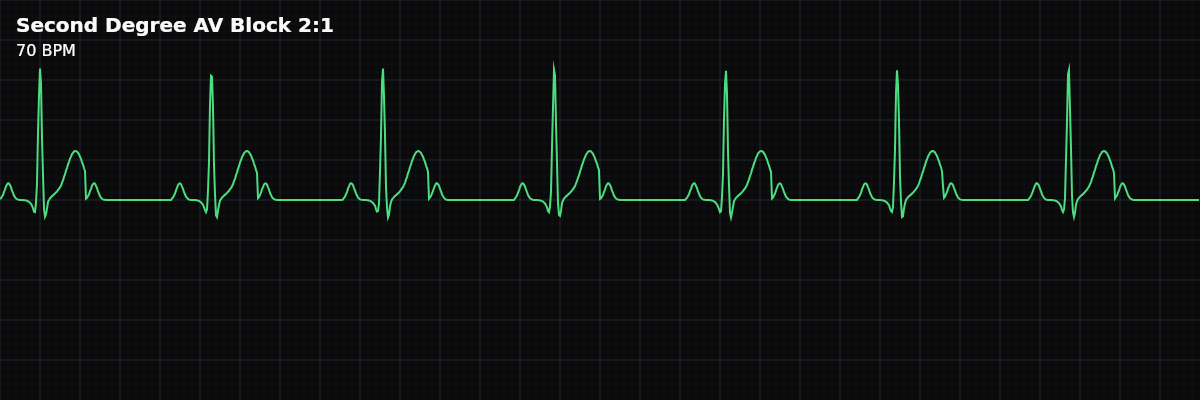
| Rate | Ventricular = half of atrial rate |
|---|---|
| Rhythm | Regular (every other P conducted) |
| P Waves | Upright, two P waves per QRS |
| PR Interval | Constant on conducted beats |
| QRS Duration | Narrow or wide (depends on block level) |
Second Degree AV Block 2:1 is the diagnostic puzzle of the AV block world. Every other P wave is blocked, producing a fixed ratio of two P waves for every one QRS complex. The problem: with only one conducted beat between each drop, you cannot see whether the PR interval was lengthening (Type I) or constant (Type II) before the dropped beat. The pattern that would tell you the type simply is not visible.
For monitor technicians, 2:1 block is important because it often produces symptomatic bradycardia — the ventricular rate is half the atrial rate. A patient with an atrial rate of 70 has a ventricular rate of only 35. The other critical skill is using the QRS width as a clue: narrow QRS suggests the block is at the AV node (more benign), while wide QRS suggests it is infranodal (more dangerous).
What Changed from Normal Sinus Rhythm
2:1 block changes two things from NSR: half the beats are dropped (every other P wave fails to conduct), and the ventricular rate is cut in half. The P waves remain normal and regular — the SA node fires on schedule. The conducted beats have a constant PR interval. The QRS width becomes the most important diagnostic clue for determining the underlying type.
Five Criteria: 2:1 AV Block vs NSR
- Rate: Half of atrial rate (often bradycardic)
- Ventricular rate is exactly 50% of atrial rate. If the atrial rate is 80, the ventricular rate is 40. This fixed halving makes the rate easy to calculate once you identify the pattern.
- Regularity: Regular (fixed conduction ratio)
- Both P-P intervals and R-R intervals are regular. The pattern is predictable: conducted beat, blocked beat, conducted beat, blocked beat. No group beating.
- P Waves: Normal, regular — twice as many as QRS complexes
- P waves march at a constant rate. For every QRS complex, there is an additional P wave that is not followed by a QRS. Count the P waves: you will find exactly twice as many as QRS complexes.
- PR Interval: Constant for conducted beats
- All conducted beats have the same PR interval. It may be normal or prolonged, but it does not vary. Since only one beat conducts between each drop, you cannot assess PR progression.
- QRS Complex: Variable — the key diagnostic clue
- Narrow QRS (<0.12s) favors AV nodal block (Type I pattern) — generally more benign. Wide QRS (>0.12s) favors infranodal block (Type II pattern) — more dangerous, higher risk of complete heart block.
What 2:1 AV Block Looks Like on the Strip
On the strip, 2:1 block has a distinctive look: a regular rhythm that seems slower than expected, with extra P waves hiding between the QRS complexes. For every QRS, there is a P wave that conducted it and another P wave sitting in the T wave or ST segment that did not conduct. The key to identification is finding those hidden non-conducted P waves — look carefully in the ST segment and T wave for bumps that are not part of the normal waveform.
Why 2:1 Cannot Be Typed from the Strip
In a 3:2 Wenckebach cycle, you see PR1 (short), PR2 (longer), then a drop — the progressive lengthening proves Type I. In a 3:1 Mobitz II, you see PR1 (constant), then two dropped beats — the constant PR proves Type II. But in 2:1, you see PR1, then a drop, then PR1, then a drop. There is only one conducted beat between drops — no pattern can emerge. The best clue from the strip alone is the QRS width: **Narrow QRS** — Favors AV nodal block (Type I mechanism). Generally more benign. **Wide QRS** — Favors infranodal block (Type II mechanism). More concerning, higher risk of progression.
Clinical Context for Monitor Technicians
2:1 AV block can occur with any cause of AV conduction disease: medications (beta-blockers, calcium channel blockers, digoxin), myocardial infarction, degenerative conduction disease, myocarditis, or post-cardiac surgery. In inferior MI, the block is usually at the AV node (more benign, often resolves). In anterior MI, the block is usually infranodal (more dangerous, often requires pacing).
When to Escalate
**Notify promptly:** - New 2:1 AV block (first documentation for this patient) - Wide QRS with 2:1 block (strongly suggests infranodal Type II — higher acuity) - Patient is symptomatic — dizziness, syncope, fatigue, hypotension - Ventricular rate below 40 BPM - Progression to higher-degree block (3:1 or complete block) **Document and monitor:** - Known, stable 2:1 block with narrow QRS and adequate ventricular rate - 2:1 block in a patient on known AV-nodal blocking medications with stable vitals