Supraventricular Tachycardia (SVT) — ECG Rhythm | Telemetric Pro
A rapid rhythm (150-250 bpm) originating above the ventricles, characterized by sudden onset and termination, where P-waves are typically absent or buried due to the extreme rate.
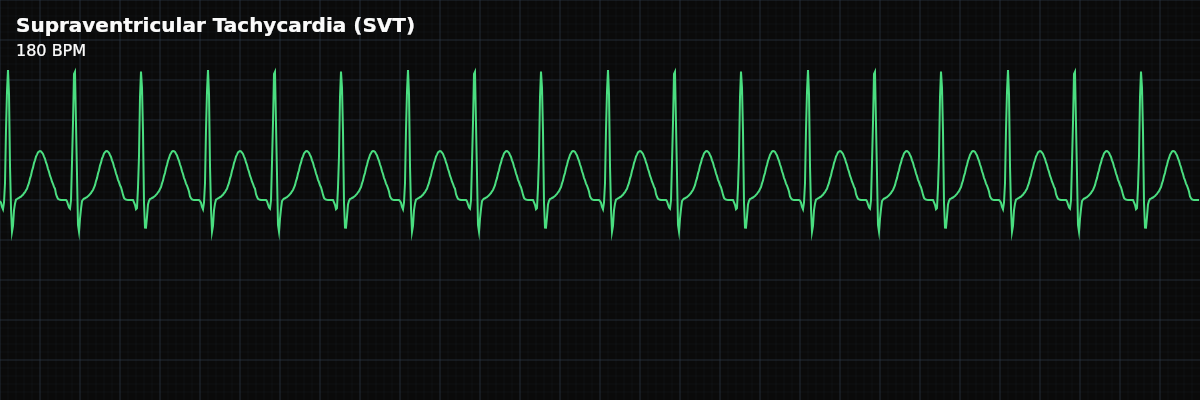
| Rate | 150–250 bpm |
|---|---|
| Rhythm | Regular |
| P Waves | Absent or hidden |
| PR Interval | Not applicable |
| QRS Duration | < 0.12 s |
Every rhythm you have studied so far — NSR, Sinus Bradycardia, Sinus Tachycardia — has one thing in common: the SA node is in control. The rate may be fast or slow, but the conduction pathway is intact and orderly. SVT is the first rhythm where that control is lost. The impulse no longer originates from the SA node in the usual way. Instead, an electrical loop takes over, driving the ventricles at rates the sinus node would never produce on its own.
This makes SVT a fundamentally different challenge on the monitor. In Sinus Tachycardia, you see a fast heart that is *responding* to something — fever, pain, dehydration. The rate rises gradually and falls gradually. SVT behaves like a light switch: one beat the rhythm is normal, the next beat the rate jumps to 180 and locks there. That sudden onset is the single most important clinical clue, and the reason SVT demands immediate attention.
What Changed from Normal Sinus Rhythm
SVT is a **multi-criteria deviation** from NSR. The rate is dramatically faster, P waves disappear, and the PR interval becomes unmeasurable. However, the QRS complex stays narrow — this is the key reassurance that ventricular conduction is normal even though the driving mechanism has changed.
Five Criteria: SVT vs Normal Sinus Rhythm
- Rate: 150-250 bpm (NSR: 60-100)
- SVT rates are dramatically faster than sinus rhythms. The typical range is 150-220 bpm in adults. Rates this fast compress the entire cardiac cycle — there is barely any isoelectric baseline between beats.
- Regularity: Perfectly regular (same as NSR)
- SVT is metronomically regular — every R-R interval is identical. This "machine-like" regularity is a hallmark of re-entry circuits and helps distinguish SVT from other rapid rhythms.
- P Waves: Absent or buried (NSR: upright, one per QRS)
- At 180+ bpm, there is not enough time between beats for a visible P wave. P waves are typically buried inside the T wave of the preceding beat, making them impossible to identify.
- PR Interval: Not measurable (NSR: 120-200ms)
- With no visible P wave, the PR interval cannot be measured. This is a direct consequence of the rate — the atrial and ventricular depolarizations overlap.
- QRS Width: Narrow, <120ms (same as NSR)
- The narrow QRS confirms that ventricular depolarization still uses the normal His-Purkinje system. This is the defining feature of "supraventricular" — the origin is above, but the ventricles conduct normally.
Rate
SVT rates typically range from 150 to 250 bpm, with most episodes landing between 150 and 220. This far exceeds the ceiling of normal sinus acceleration. A rate of 180 bpm means each cardiac cycle completes in about a third of a second — barely enough time for the chambers to fill before the next contraction.
Regularity
SVT is perfectly regular — every R-R interval is identical. This precision comes from the re-entry circuit itself: the loop has a fixed path length and conduction velocity, so each trip around the circuit takes exactly the same amount of time. Compare this to Sinus Tachycardia, which has subtle beat-to-beat variability because the SA node responds to continuous autonomic input.
P Waves
In SVT, P waves are typically **absent or buried**. This is not because the atria have stopped depolarizing — they are still contracting. The problem is timing: at 180 bpm, atrial depolarization occurs simultaneously with ventricular repolarization. The P wave hides inside the T wave of the preceding beat, making it invisible on the strip.
QRS Complex
The QRS in SVT is narrow (<120ms) because the re-entry circuit sits above the ventricles. Once the impulse exits the circuit and reaches the His bundle, it travels through the normal Purkinje fibers — the same pathway used in NSR. The ventricles depolarize quickly and symmetrically, producing a narrow QRS identical in morphology to the patient's baseline.
SVT vs Sinus Tachycardia: The Critical Distinction
This is the comparison you will make most often at the monitor. Both rhythms are fast, regular, and narrow — but they have fundamentally different causes and urgency levels.
**Onset** is the strongest differentiator. Sinus Tachycardia ramps up gradually over seconds to minutes — the rate climbs from 80 to 100 to 120 as the body responds to a stressor. SVT switches on instantly. One beat is 75, the next is 180. If your monitor's trend graph shows a sudden vertical jump in heart rate, think SVT. **P waves** are the strip-level differentiator. In Sinus Tachycardia, P waves are present before every QRS — they may be harder to see at faster rates, but they are there. In SVT, P waves disappear entirely or hide inside the T wave. **Rate range** provides a clue but not a rule. Sinus Tachycardia rarely exceeds 150 bpm in a resting adult. SVT typically runs 150-220 bpm. A rate above 150 with no visible P waves strongly suggests SVT.