Ventricular Fibrillation (VFib) — ECG Rhythm | Telemetric Pro
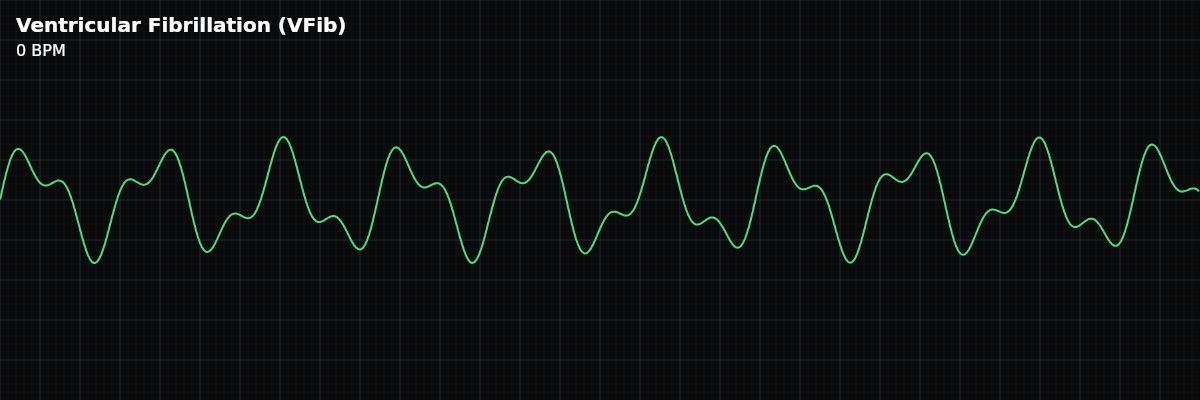
A chaotic, life-threatening cardiac arrest rhythm where the ventricles quiver without any effective contraction, resulting in zero cardiac output.
| Rate | Undeterminable |
|---|---|
| Rhythm | Chaotic, no organized pattern |
| P Waves | Absent |
| PR Interval | Not applicable |
| QRS Duration | No identifiable QRS complexes |
Ventricular Fibrillation is cardiac arrest. There is no equivocation, no "it depends," no wait-and-see. The moment VFib appears on the monitor, the patient has no pulse, no cardiac output, and no blood reaching the brain. Without immediate intervention, brain death begins within minutes.
VFib is also the most visually distinctive rhythm you will ever see. Every other rhythm — no matter how abnormal — has identifiable waveforms: P waves, QRS complexes, T waves, or some combination. VFib has none of these. The tracing is pure chaos: random, irregular oscillations with no repeating pattern. Nothing on the strip can be measured, counted, or named.
What Changed from Normal Sinus Rhythm
VFib is not a deviation from NSR — it is the complete destruction of organized cardiac electrical activity. There is no rate to measure, no rhythm to classify, no waveforms to identify. Every criterion from the five-criteria method is "absent" or "not applicable." The strip tells you one thing: this patient is in cardiac arrest.
What VFib Looks Like on the Strip
The tracing consists of random, irregular deflections above and below the baseline. The morphology changes continuously — no two oscillations look the same. There are no organized waveforms to label, no intervals to measure, no rate to calculate. The heart is not contracting; it is quivering.
Coarse VFib, Fine VFib, and What the Terms Mean
Many textbooks and training courses describe VFib as either "coarse" or "fine" based on the amplitude of the fibrillatory waves: - **Coarse VFib** — larger, more visible chaotic oscillations, generally greater than 3 mm at standard calibration - **Fine VFib** — small, low-amplitude oscillations barely deviating from the baseline, generally less than 3 mm These terms are widely used in clinical practice, and you will hear them during codes and in documentation. However, there are important caveats every monitor technician should understand.
**The coarse/fine distinction is subjective.** There is no universally standardized scientific threshold that separates coarse from fine VFib. The commonly cited 3 mm cutoff is a teaching convention, not an AHA-endorsed diagnostic criterion. Individual providers make this determination by visual inspection, and different clinicians may classify the same strip differently. **Treatment does not change based on amplitude.** Per AHA 2025 and ERC 2025 guidelines, the ACLS cardiac arrest algorithm is identical for all VFib regardless of wave size. Coarse or fine, VFib is always a shockable rhythm requiring immediate defibrillation. Do not delay treatment to assess amplitude. **Amplitude reflects time and myocardial energy.** Research supports the Weisfeldt three-phase model of cardiac arrest: VFib tends to start with larger amplitude (the "electrical phase," first 4-5 minutes) and degrade to lower amplitude as the myocardium depletes its energy reserves. Coarse VFib generally appears earlier in arrest; fine VFib generally appears later. CPR can partially restore coronary perfusion and increase VFib amplitude — one reason high-quality chest compressions are critical. **Higher amplitude is associated with better outcomes.** Studies (Callaway et al., 2018; Ristagno et al., 2014) have found that higher-amplitude VFib before defibrillation correlates with greater likelihood of return of spontaneous circulation (ROSC). However, this is a population-level association — it does not mean fine VFib should not be shocked. All VFib is shockable. Always.