Atrial Tachycardia — ECG Rhythm | Telemetric Pro
A supraventricular tachycardia originating from an ectopic atrial focus outside the SA node, producing abnormal P waves at rates of 130-250 BPM with the AV node acting as a passive bystander.
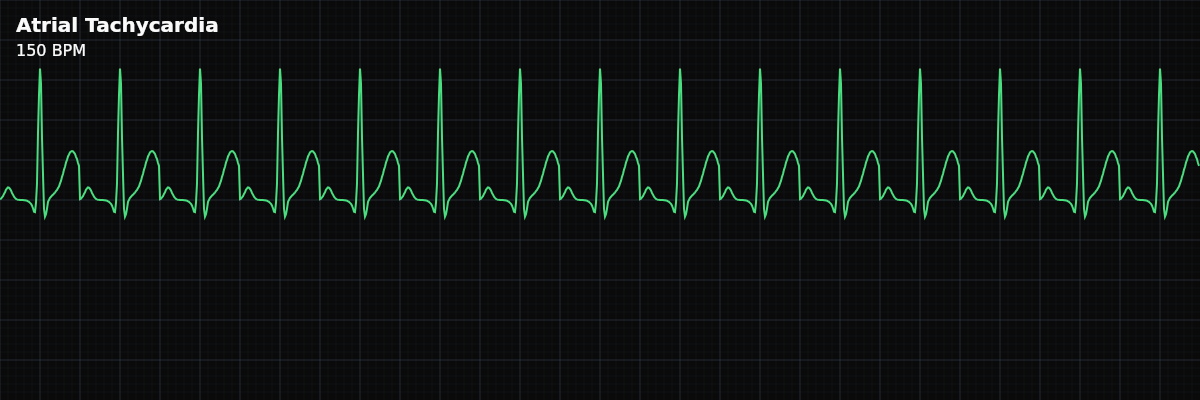
| Rate | 130–250 bpm |
|---|---|
| Rhythm | Regular |
| P Waves | Present but abnormal morphology |
| PR Interval | Normal or short |
| QRS Duration | < 0.12 s |
Atrial Tachycardia is what happens when a spot in the atrial tissue decides to become the pacemaker — and fires faster than the SA node. This ectopic focus generates rapid impulses at 130-250 BPM, and because it is located somewhere other than the SA node, the P waves look different from normal sinus P waves.
For monitor technicians, the most important thing about atrial tachycardia is that it has visible P waves — unlike SVT (where P waves are often hidden) and atrial flutter (where P waves are replaced by sawtooth F waves). The P waves look abnormal, but they are there. This is your primary clue. The second critical feature is that the AV node is not part of the circuit, so AV block can occur without stopping the tachycardia.
What Changed from Normal Sinus Rhythm
Atrial tachycardia changes two things from NSR: the rate (much faster) and the P-wave morphology (different shape because the impulse originates from a different location). The conduction pathway through the AV node and ventricles remains normal, so the QRS complex is narrow and unchanged.
Five Criteria: Atrial Tachycardia vs NSR
- Rate: 130-250 BPM (atrial)
- The atrial rate is 130-250 BPM. The ventricular rate depends on AV conduction — with 1:1 conduction, the ventricular rate equals the atrial rate. With 2:1 block, the ventricular rate is half.
- Regularity: Usually regular
- The atrial rhythm is regular (each ectopic impulse fires at the same interval). The ventricular rhythm is regular with fixed AV conduction, or irregular if the conduction ratio varies.
- P Waves: Present but abnormal morphology
- P waves are visible with isoelectric baseline between them. Their shape differs from sinus P waves because the impulse originates from a different atrial location. They may be partially hidden in the preceding T wave at fast rates.
- PR Interval: Normal or slightly variable
- The PR interval may be normal if the ectopic focus is near the SA node area, or slightly different if the focus is elsewhere in the atria. It remains constant beat-to-beat with fixed conduction.
- QRS Complex: Narrow (<0.12s)
- Ventricular conduction is normal — the impulse travels through the AV node and His-Purkinje system normally. QRS morphology is identical to NSR.
What Atrial Tachycardia Looks Like on the Strip
On the strip, atrial tachycardia shows a rapid, regular narrow-complex rhythm with visible P waves that look different from the patient's normal sinus P waves. At faster rates, the P waves may be partially buried in the preceding T wave, making them harder to spot. Look for a notch or deformity in the T wave that was not present in slower rhythms — that may be a hidden ectopic P wave.
The AV Block Test: What Makes AT Unique
The single most important feature that separates atrial tachycardia from other SVTs is how it responds to AV block: **Atrial Tachycardia** — AV block can occur (naturally or with medication) without terminating the rhythm. The P waves continue at the same rate even though some are not conducted to the ventricles. This proves the AV node is not part of the circuit. **AVNRT / AVRT** — AV block terminates the rhythm immediately. These rhythms require the AV node as part of their re-entry circuit, so blocking the AV node breaks the circuit and stops the tachycardia.
Atrial Tachycardia vs Sinus Tachycardia
Both are rapid rhythms with visible P waves, but: **Sinus Tachycardia** — P waves look identical to the patient's normal sinus P waves (upright in II, inverted in aVR). Rate usually 100-160 BPM. Rate changes gradually in response to activity, pain, or physiologic stress. **Atrial Tachycardia** — P waves look different from the patient's normal sinus P waves (morphology depends on ectopic focus location). Rate can exceed 200 BPM. Onset is often abrupt (especially re-entrant types) or shows warm-up pattern (automatic types).
Clinical Context for Monitor Technicians
Atrial tachycardia can occur in patients with structural heart disease, post-cardiac surgery (scar-related), COPD, or digoxin use. It accounts for roughly 10% of SVT cases. Unlike AVNRT (which typically occurs in young, otherwise healthy patients), atrial tachycardia more commonly has an underlying cardiac or systemic cause.
Digoxin Toxicity and Atrial Tachycardia
Digoxin is a medication used to control heart rate — but at toxic levels, it paradoxically causes arrhythmias. The mechanism is twofold: digoxin enhances atrial automaticity (making ectopic foci fire faster) while simultaneously depressing AV node conduction (slowing ventricular response). The result is a fast atrial rate paired with a slow or blocked ventricular rate — atrial tachycardia with AV block. This pattern is one of the most recognizable toxicity signatures on the monitor. What you see is rapid P waves marching along at the atrial rate, but the QRS complexes are fewer — some P waves are not conducted. The atrial rhythm is regular and fast, but the ventricular rhythm is slow and may have varying conduction ratios (2:1, 3:1, or Wenckebach patterns).