Wandering Atrial Pacemaker (WAP) — ECG Rhythm | Telemetric Pro
An irregular rhythm with at least 3 distinct P-wave morphologies at a rate below 100 BPM, indicating the dominant pacemaker is shifting between the SA node and other atrial foci.
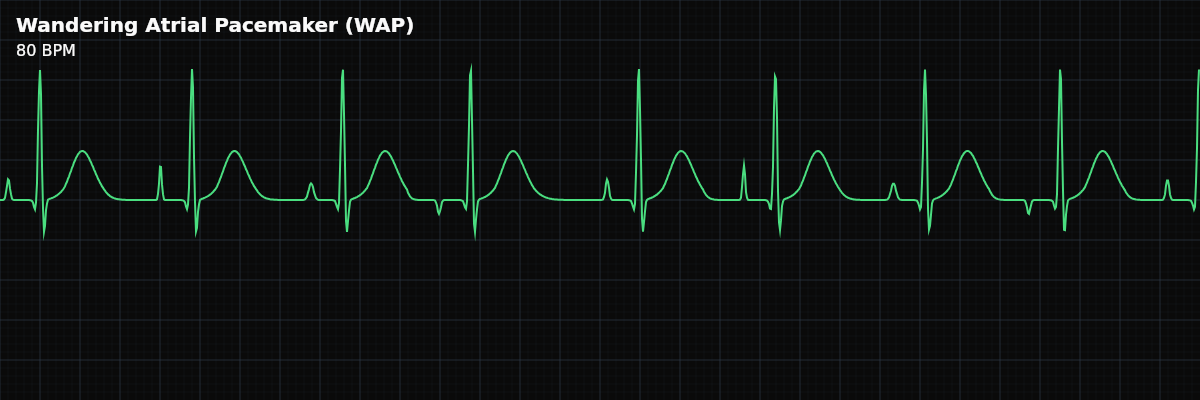
| Rate | < 100 bpm (typically 60–100) |
|---|---|
| Rhythm | Irregularly irregular |
| P Waves | At least 3 distinct morphologies |
| PR Interval | Variable |
| QRS Duration | < 0.12 s |
Wandering Atrial Pacemaker is what happens when the dominant pacemaker can't make up its mind. Instead of the SA node maintaining control, the pacemaker focus shifts — sometimes it fires from the SA node, sometimes from a spot in the left atrium, sometimes from near the AV node. Each shift produces a different P-wave morphology, because the depolarization wave takes a different path through the atria.
For monitor technicians, WAP is worth knowing for two reasons. First, it is usually benign — common in young people, athletes, and during sleep — so recognizing it prevents unnecessary escalation. Second, it can be mistaken for AFib (both are irregular), and the distinction matters because the clinical implications are very different.
What Changed from Normal Sinus Rhythm
WAP changes three things from NSR: the P-wave morphology (multiple shapes as the focus shifts), the PR interval (variable with each shift), and the regularity (irregularly irregular because each focus fires at its own timing). The QRS remains narrow — ventricular conduction is normal regardless of where the atrial impulse originates.
Five Criteria: WAP vs NSR
- Rate: <100 BPM (typically 60-100)
- Must be below 100 BPM by definition. If the rate exceeds 100 BPM with the same multi-morphology P-wave pattern, the rhythm is reclassified as Multifocal Atrial Tachycardia (MAT).
- Regularity: Irregularly irregular
- Both PP and RR intervals vary unpredictably as the pacemaker shifts between foci. No predictable pattern to the irregularity.
- P Waves: At least 3 distinct morphologies
- The diagnostic hallmark. At least 3 different P-wave shapes must be visible, each representing a different pacemaker site. Some may be upright, some inverted, some biphasic.
- PR Interval: Variable
- Changes from beat to beat as the pacemaker focus shifts. Shorter PR when the focus is near the AV junction, longer PR when it is higher in the atria.
- QRS Complex: Narrow (<0.12s)
- Ventricular conduction is normal. The QRS morphology is the same regardless of which atrial focus generated the impulse.
What WAP Looks Like on the Strip
On the strip, WAP looks like an irregular rhythm where the P waves keep changing shape. Compare the P wave before each QRS complex — you should see at least 3 distinctly different morphologies. Some P waves may be tall and upright, others flat or inverted, others biphasic. The PR interval changes with the P-wave morphology. Between P waves, the baseline is flat and isoelectric.
WAP vs Sinus Arrhythmia
Both are irregular sinus-rate rhythms that are often benign, but they are fundamentally different: **Wandering Atrial Pacemaker** — P-wave morphology changes from beat to beat (multiple foci). PR interval is variable. The pacemaker is shifting between the SA node and other atrial sites. **Sinus Arrhythmia** — P-wave morphology is uniform throughout (single focus — SA node). PR interval is constant. Only the timing (RR interval) varies with respiration.
WAP vs Atrial Fibrillation
Both are irregularly irregular, and both can occur at similar rates: **WAP** — Discrete P waves are present (at least 3 morphologies). Isoelectric baseline between P waves. Each QRS is preceded by a P wave. Rate <100 BPM. **AFib** — No discrete P waves. Wavy, fibrillatory baseline. QRS complexes appear without organized atrial activity. Rate can be any range.
Clinical Context for Monitor Technicians
WAP is most common in young, healthy individuals with high vagal tone — athletes, children, and anyone during deep sleep. In these populations, it is a normal variant and requires no treatment. In elderly patients, new-onset WAP may indicate SA node dysfunction and warrants evaluation.
Electrolyte and Medication Context
The same electrolyte context that applies to MAT applies to WAP. Low potassium (hypokalemia) and low magnesium (hypomagnesemia) increase atrial irritability, making it easier for multiple foci to fire. When K+ and Mg2+ are repleted, the wandering pacemaker pattern may normalize — the P-wave morphologies may consolidate as the SA node regains consistent dominance. COPD medications — particularly albuterol nebulizers and theophylline — can contribute to multiple atrial foci by stimulating beta-adrenergic receptors in atrial tissue. In patients receiving frequent bronchodilator treatments, the medication may be partly responsible for the shifting pacemaker. WAP is generally less clinically urgent than MAT since the rate is below 100 BPM, but the same underlying causes apply. The difference is one of degree — the atria are irritated enough to produce multiple foci but not so much that the rate exceeds 100. If the underlying cause worsens, WAP can accelerate into MAT.