ST Elevation (STEMI Pattern) — ECG Rhythm | Telemetric Pro
Marked ST segment elevation above the baseline, indicating acute transmural myocardial injury — the full thickness of the heart wall is ischemic. This pattern represents a medical emergency requiring immediate reperfusion.
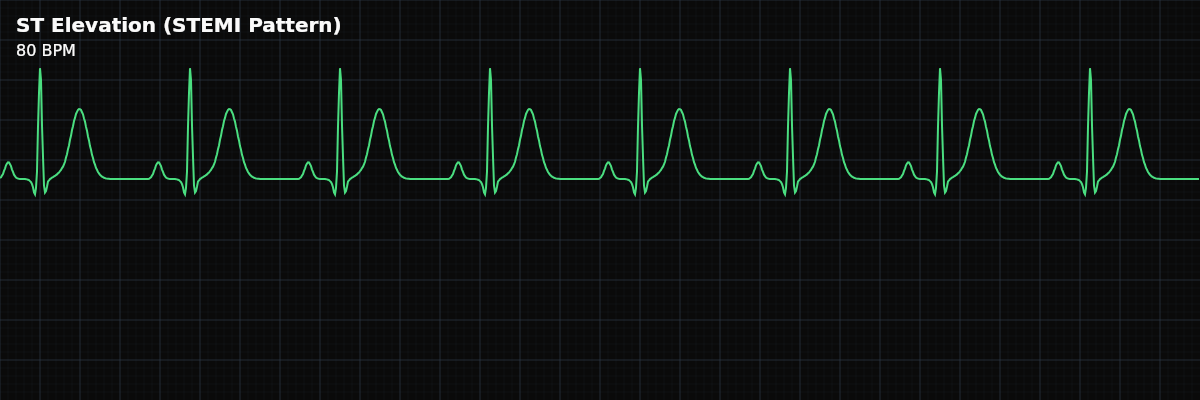
| Rate | 60–100 bpm (underlying sinus) |
|---|---|
| Rhythm | Regular (underlying sinus) |
| P Waves | Upright, one before each QRS |
| PR Interval | 0.12–0.20 s |
| QRS Duration | < 0.12 s |
ST Elevation is the ECG hallmark of acute transmural myocardial injury — typically caused by complete occlusion of a coronary artery. When the full thickness of the heart wall loses its blood supply, the ST segment rises above the baseline in the leads facing the injured area. This is a time-critical emergency: the longer the artery stays occluded, the more heart muscle dies.
For monitor technicians, recognizing ST elevation is one of the most impactful skills you can develop. Rapid identification of ST elevation triggers the chain of events — emergency notification, cath lab activation, and reperfusion — that saves heart muscle and lives. On the monitor, you may be the first person to see the ST segment change.
What Changed from Normal
Like ST depression, this is a morphology change — the underlying rhythm is usually normal sinus. The P waves, PR interval, and QRS are unchanged. Only the ST segment is affected, rising above where it should be. The elevation may be accompanied by reciprocal ST depression in opposite leads.
What to Look For
- ST Segment: Elevated above baseline
- The ST segment rises above the isoelectric line after the QRS. Significant elevation: >=1mm in limb leads, >=2mm in precordial leads (V2-V3).
- Distribution: Contiguous leads
- STEMI criteria require elevation in two or more contiguous leads (leads that look at the same area). The lead pattern localizes the territory.
- Reciprocal Changes: ST depression in opposite leads
- ST depression in leads opposite to the elevation strongly supports acute MI. For example, inferior STEMI (II, III, aVF elevation) often shows reciprocal depression in I and aVL.
- Evolution: Changes over time
- Acute STEMI evolves: ST elevation appears first, then T wave inversion, then Q waves develop. On the monitor, you are looking for the earliest change — the ST elevation itself.
What ST Elevation Looks Like on the Strip
On the monitor, ST elevation appears as the segment after the QRS rising above the baseline — the T wave seems to "merge upward" with the QRS rather than returning to baseline first. In dramatic cases, the ST segment and T wave form a single upward curve (tombstone pattern). Compare to the patient's baseline — any new elevation is significant.
Localization by Lead Distribution
The leads showing ST elevation tell you which part of the heart is injured: **Anterior (V1-V4)** — LAD artery territory. Highest mortality. The anterior wall of the left ventricle. **Inferior (II, III, aVF)** — Usually RCA territory. Check for RV involvement. The inferior wall. **Lateral (I, aVL, V5-V6)** — Circumflex or diagonal branch. Often accompanies other territories. **Posterior** — Not directly visible on standard leads. Look for reciprocal ST depression in V1-V3.
Clinical Context for Monitor Technicians
While STEMI from coronary occlusion is the most critical cause of ST elevation, other conditions can mimic the pattern: pericarditis (diffuse elevation, no reciprocal changes), early repolarization (benign variant in young patients), left ventricular hypertrophy, LBBB, and ventricular paced rhythms. The clinical team will differentiate these — your role is to identify the ST change and escalate.
When to Escalate
**Notify immediately:** - New ST elevation with chest pain (possible STEMI — time-critical emergency) - New ST elevation without symptoms (silent ischemia) - Dynamic ST elevation (comes and goes — may indicate vasospasm) - ST elevation during a procedure or hemodynamic instability **Notify promptly:** - Gradual ST changes from baseline ST elevation with symptoms is never a "document and monitor" finding. Always escalate immediately.
Post-Identification Timeline
Once ST elevation is identified and a STEMI alert is called, the clock starts. The sequence is rapid: STEMI alert notification, cath lab activation, and emergent PCI (percutaneous coronary intervention) — a catheter-based procedure to open the blocked artery. The goal is "door-to-balloon" time under 90 minutes. During the rush to the cath lab, the tech's responsibilities do not stop. Print the clearest strip showing the ST elevation changes, document the time you first identified the ST changes, and continue monitoring the rhythm for arrhythmias during transport and cath lab preparation.