ST Depression (Ischemia) — ECG Rhythm | Telemetric Pro
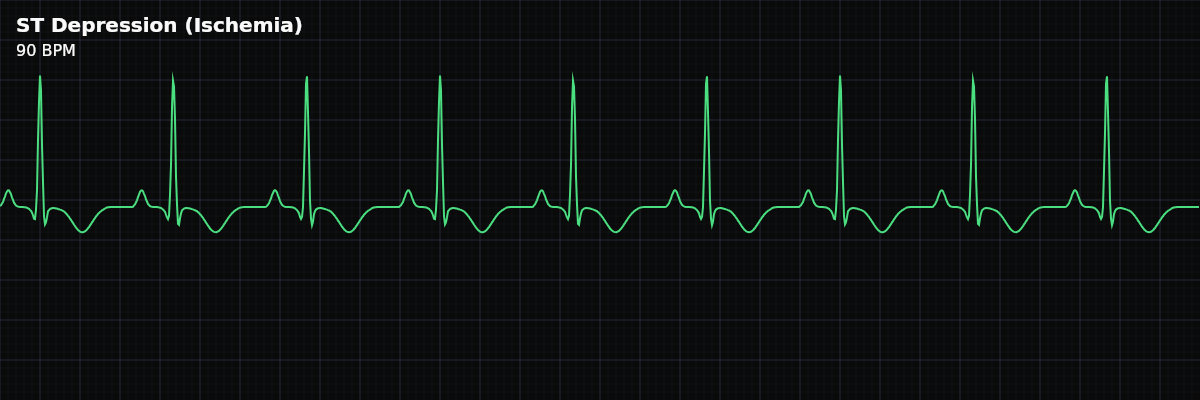
ST segment depression below the baseline, indicating subendocardial ischemia — the inner layer of the heart wall is not receiving enough oxygen. This is an ST segment change, not a rhythm disturbance.
| Rate | 60–100 bpm (underlying sinus) |
|---|---|
| Rhythm | Regular (underlying sinus) |
| P Waves | Upright, one before each QRS |
| PR Interval | 0.12–0.20 s |
| QRS Duration | < 0.12 s |
ST Depression is not a rhythm — it is a morphology change that indicates the heart muscle is not getting enough oxygen. The ST segment, which is normally flat and at the baseline, drops below the baseline. This depression signals that the inner layer of the heart wall (subendocardium) is ischemic: oxygen demand is exceeding supply.
For monitor technicians, ST depression is a critical finding to recognize and report. On the monitor, you may see the ST segment dipping below the baseline in real time — especially during episodes of chest pain, tachycardia, or hemodynamic stress. Your role is to identify the change, compare to the patient's baseline, and notify the clinical team.
What Changed from Normal
The underlying rhythm does not change — the P waves, PR interval, and QRS are normal. Only the ST segment is affected. The depression may come and go (dynamic ST changes) as ischemia waxes and wanes, which is why continuous monitoring is valuable.
Types of ST Depression
- Downsloping — Most specific for ischemia
- The ST segment slopes downward from the J point. This morphology has the highest correlation with coronary artery disease and is the most concerning pattern.
- Horizontal — Also concerning for ischemia
- The ST segment runs parallel to the baseline below it. Nearly as specific as downsloping for ischemia, especially when measured at 60-80ms after the J point.
- Upsloping — Least specific
- The ST segment slopes upward after the J point. May be a normal variant during exercise or tachycardia. Less reliably indicates ischemia but still warrants clinical evaluation.
What ST Depression Looks Like on the Strip
On the monitor, ST depression appears as the segment after the QRS dipping below the baseline. Compare the current ST segment to the patient's baseline — if it was flat at the baseline before and is now depressed, that is a new change worth reporting. Dynamic changes (ST depression that comes and goes with symptoms) are particularly significant.
Clinical Context for Monitor Technicians
ST depression can result from many conditions: acute coronary syndrome (NSTEMI, unstable angina), reciprocal changes opposite to STEMI, demand ischemia (tachycardia, anemia, hypotension), digoxin effect (characteristic "scooped" morphology), left ventricular hypertrophy, hypokalemia, and rate-related changes during tachycardia.
Demand Ischemia
Tachycardia can cause ST depression without any coronary artery occlusion. When the heart rate climbs, the heart muscle needs more oxygen — but the faster rate also shortens diastole, which is when the coronary arteries fill. If the rate increases enough, oxygen demand exceeds what the coronary arteries can supply, producing ST depression. This is called "demand ischemia" or rate-related ST changes. It is especially common in patients with preexisting coronary artery disease, but can occur in anyone at extreme heart rates.
If you see ST depression that appeared after a rate increase (patient got agitated, developed SVT, etc.), include the rate and timing in your report. Rate-related ST changes often resolve when the rate normalizes.
Going Deeper — STEMI Equivalents That Look Like ST Depression
Some patterns present with ST depression or T-wave changes — not classic ST elevation — but indicate acute coronary occlusion requiring emergent intervention. These are "STEMI equivalents" and should not be dismissed as routine ischemia.
What Happens When Treatment Works
For demand ischemia, rate control is the treatment. As the heart rate comes down — after a beta-blocker, calcium channel blocker, or other rate-control intervention — the ST depression should gradually resolve as oxygen supply catches up with demand. Print comparison strips before and after rate control to document the response. For vasospastic ischemia (Prinzmetal's angina), nitroglycerin can produce a dramatic response — the ST changes may resolve within minutes as the coronary artery spasm relaxes and blood flow is restored.
Medication Context
Several medications can produce ST changes on the monitor that are not ischemia. Digoxin causes a characteristic "scooped" ST depression — a gradual downward curve that looks like an inverted checkmark. This is the digoxin effect, not ischemia, and is an expected finding in patients taking the drug. Beta-blockers, while generally reducing ST changes by lowering heart rate, may in rare cases unmask a Brugada pattern in susceptible patients — a coved ST elevation in V1-V2 that indicates an inherited arrhythmia syndrome.