Pacemaker Undersensing (Failure to Sense) — ECG Rhythm | Telemetric Pro
A pacemaker malfunction where the device does not detect (sense) the heart’s native electrical activity. The pacemaker fires when it should not, delivering pacing spikes into native QRS complexes or T waves because it does not "see" them.
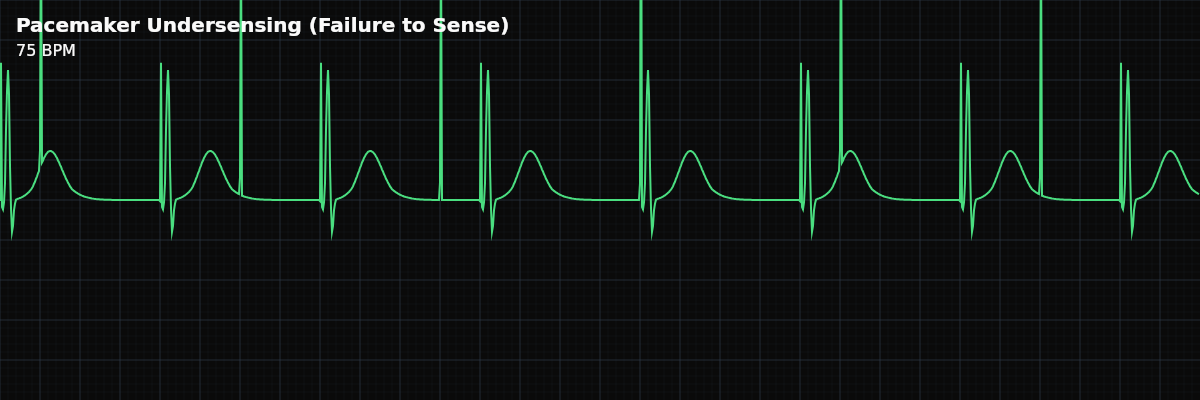
Pacemaker undersensing means the pacemaker is not detecting the heart’s own electrical activity. A properly functioning demand pacemaker senses native cardiac beats and withholds its pacing spike when the heart is beating on its own. When undersensing occurs, the pacemaker is blind to native activity — it fires pacing spikes as if no native beats are happening, delivering stimuli at inappropriate times.
For monitor technicians, undersensing is critical to recognize because pacing spikes can land on vulnerable parts of the cardiac cycle. A spike falling on a T wave is the pacemaker equivalent of the R-on-T phenomenon — it can trigger ventricular fibrillation. Even when spikes do not land on T waves, the competition between the pacemaker and the heart’s own rhythm creates a dangerous situation where two electrical sources are fighting for control of the ventricles.
What Undersensing Looks Like on the Strip
The hallmark of undersensing is pacing spikes appearing when they should not. In a properly sensing pacemaker, the device detects native beats and withholds its output. In undersensing, the pacemaker fires on schedule — at its programmed rate — regardless of what the heart is doing: **Spikes falling on or near QRS complexes** — The pacemaker does not see the native QRS, so it fires a spike into it. **Spikes falling on ST segments** — The pacemaker fires during the plateau phase of repolarization. **Spikes falling on T waves** — The most dangerous finding. The T wave is the vulnerable period, and a spike here can trigger ventricular fibrillation.
Why Undersensing Is Dangerous
Undersensing creates a competition between two electrical sources: the heart’s native conduction system and the pacemaker. Both are trying to depolarize the ventricles, but they are not coordinated. This competition carries two primary risks: **1. R-on-T equivalent** — A pacing spike landing on the T wave delivers an electrical stimulus during the vulnerable period of repolarization. This can trigger ventricular fibrillation, just as a PVC landing on a T wave can. The pacemaker spike, though small, may be sufficient to trigger a re-entrant circuit. **2. Hemodynamic compromise** — When pacing spikes compete with native beats, the timing of ventricular contraction becomes chaotic. The ventricles may receive competing stimuli, leading to inefficient contraction and reduced cardiac output.
Atrial Undersensing vs Ventricular Undersensing
**Atrial undersensing** — The pacemaker does not detect native P waves (atrial activity). Atrial pacing spikes fire into native P waves or during the atrial refractory period. While less immediately dangerous than ventricular undersensing, it disrupts AV timing and can reduce cardiac output. **Ventricular undersensing** — The pacemaker does not detect native QRS complexes (ventricular activity). Ventricular pacing spikes fire into native QRS complexes, ST segments, or T waves. This is the more dangerous form because of the VFib risk from spikes on T waves. On the strip, ventricular undersensing is easier to identify because the native QRS and the misplaced pacing spike are both large, visible signals. Atrial undersensing may be subtle because P waves are smaller.
Sensitivity Threshold (Brief Overview)
The pacemaker’s sensitivity setting determines how large a signal the device must detect to count as a native beat. A lower sensitivity value (e.g., 1 mV) means the pacemaker is more sensitive — it will detect smaller signals. A higher sensitivity value (e.g., 5 mV) means the pacemaker requires a larger signal to sense. Undersensing occurs when the native cardiac signal is smaller than the sensitivity threshold — the pacemaker cannot see it. This can happen because the lead has shifted position, scar tissue has formed at the lead tip, the native signal is genuinely small (as in some patients with cardiomyopathy), or the sensitivity setting is programmed too high. You do not need to know the technical details of sensitivity programming. What matters is understanding the concept: the pacemaker has a threshold for what it considers a real heartbeat, and undersensing means native beats are falling below that threshold.