Pacemaker Failure to Output — ECG Rhythm | Telemetric Pro
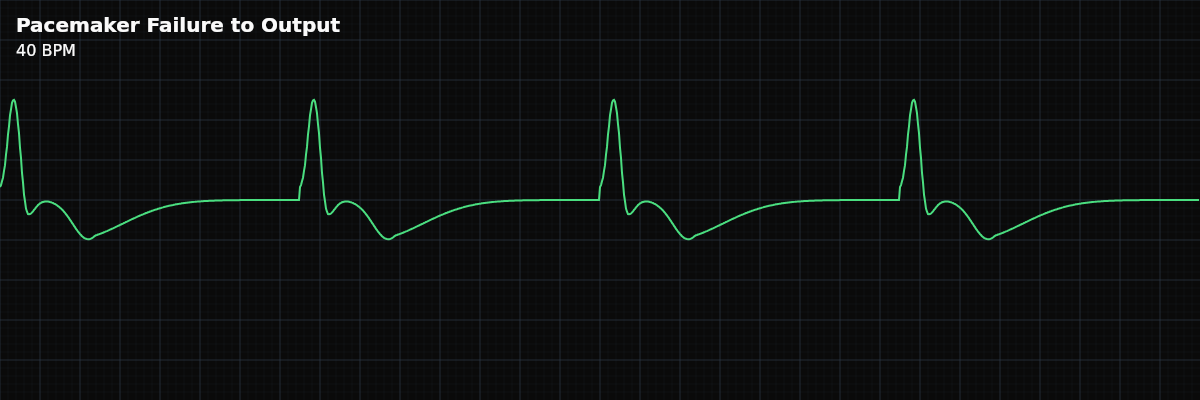
A pacemaker malfunction where the device does not fire when expected — the pacing spike itself is absent. The pacemaker is not delivering any stimulus to the heart.
| Rate | Variable (often slow/absent) |
|---|---|
| Rhythm | Irregular (expected spikes absent) |
| P Waves | No pacing spikes where expected |
| PR Interval | Not applicable |
| QRS Duration | Variable (depends on escape rhythm) |
Pacemaker failure to output means the pacemaker is not firing at all. No spike, no stimulus, no pacing. The strip shows whatever the patient's intrinsic rhythm is — often a dangerously slow escape rhythm — without any pacing artifacts. The pacemaker has essentially stopped working.
For monitor technicians, failure to output is particularly dangerous because it can look like many other slow rhythms if you are not expecting pacing. The key is knowing that the patient has a pacemaker and recognizing that spikes should be present but are not. In a pacemaker-dependent patient, failure to output can cause immediate asystole without warning.
What Changed from Normal Pacemaker Function
In normal pacemaker function, the device fires on schedule (spikes visible) whenever the native rate drops below the programmed rate. In failure to output, the device does not fire even when the rate drops below the programmed limit. The strip shows an unexpectedly slow rhythm without pacing artifacts.
Five Criteria: Failure to Output
- Rate: Slow (intrinsic rhythm only)
- Only the patient's intrinsic rhythm is present — no pacing support. May see escape rhythms (junctional 40-60, ventricular 20-40) or asystole if no escape exists.
- Regularity: Variable
- Depends entirely on the intrinsic rhythm. May be regular (escape rhythm) or irregular (pauses, intermittent failure).
- Pacing Spikes: ABSENT (the pacemaker is NOT firing)
- This is the defining feature. Expected pacing spikes are missing during periods when the pacemaker should fire (heart rate below programmed rate). The pacemaker is not delivering any stimulus.
- Pauses: Present when pacing fails
- Long pauses appear where pacing spikes should have occurred. The pause continues until an intrinsic escape beat occurs or the device resumes firing.
- Key Distinction: No spikes at all vs spikes without response
- Failure to output = no spikes. Failure to capture = spikes present but no response. This distinction is critical because the causes and urgency are different.
What Failure to Output Looks Like on the Strip
On the strip, failure to output looks like whatever the patient's underlying rhythm is — minus the pacing support. You may see a slow junctional or ventricular escape rhythm, or simply long pauses where pacing spikes should appear. The absence of spikes when the rate drops below the programmed pacing rate is diagnostic. Compare to the patient's previous strips where pacing spikes were present.
Appropriate Inhibition vs True Failure to Output
Not every absence of pacing spikes is a malfunction. In demand pacing modes (VVI, DDD), the pacemaker correctly inhibits when it senses native cardiac activity above the programmed rate: **Appropriate inhibition** — Native rate is above the programmed lower rate limit. The pacemaker is correctly holding back. The patient has an adequate heart rate. This is normal. **True failure to output** — Native rate is BELOW the programmed rate, and the pacemaker is NOT firing. The heart rate is inappropriately slow. This is a malfunction.
Clinical Context for Monitor Technicians
Common causes of failure to output include: battery depletion (end of life), lead fracture (complete break in the conductor), oversensing (device inhibited by T waves, muscle artifact, or electromagnetic interference), loose connection (at the header or lead-generator interface), circuit failure (internal component malfunction), and accidental deactivation (magnet or programming change).
Oversensing Deep-Dive
Oversensing is the most common reversible cause of failure to output. The pacemaker detects non-cardiac electrical signals and interprets them as native heartbeats, so it inhibits pacing when it should be firing. Three main categories: **T-wave oversensing** — The pacemaker mistakes the T wave for a QRS complex and resets its timing. Result: inappropriate pauses after beats with large T waves. The device "sees" a beat (the T wave), waits the programmed interval, then fires — but by then another native beat may have occurred, so the cycle repeats. More common in VVI mode because the ventricular channel has only one electrogram to interpret. **Myopotential oversensing** — Skeletal muscle activity generates electrical signals that the pacemaker interprets as cardiac activity. Shivering, hiccups, pectoral muscle contractions, and arm movements on the side of the generator can all produce myopotentials large enough to inhibit pacing. The pattern is characteristic: pauses that correlate with specific patient activities. **EMI oversensing** — Electromagnetic interference from external sources. Electric razors held near the generator, electrocautery during surgery, electric hospital beds, and MRI (in non-MRI-conditional devices) can all generate signals the pacemaker reads as cardiac activity. The result is temporary inhibition that resolves when the source is removed.