Pacemaker Failure to Capture — ECG Rhythm | Telemetric Pro
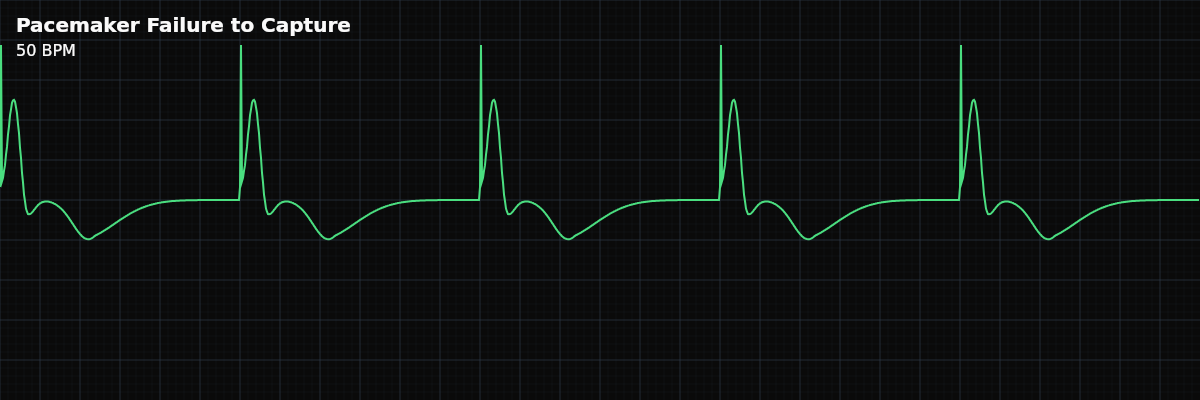
A pacemaker malfunction where the pacing spike fires but fails to produce myocardial depolarization. Spikes are visible on the strip but are not followed by the expected P wave or QRS complex.
| Rate | Variable (may be bradycardic) |
|---|---|
| Rhythm | Irregular (spikes without capture) |
| P Waves | Pacing spikes present but not followed by depolarization |
| PR Interval | Not applicable |
| QRS Duration | Variable (captured vs non-captured beats) |
Pacemaker failure to capture means the pacemaker is trying to work — the spike fires on schedule — but the electrical impulse is not strong enough to depolarize the heart muscle. The spike appears on the strip, but nothing happens after it. No P wave (if atrial pacing), no QRS (if ventricular pacing). The myocardium does not respond.
For monitor technicians, failure to capture is one of the two critical pacemaker malfunctions you must recognize immediately (the other being failure to output). The distinction is simple: in failure to capture, you SEE the spikes but they do not produce a response. In failure to output, the spikes themselves are MISSING. Failure to capture in a pacemaker-dependent patient is a life-threatening emergency.
What Changed from Normal Pacemaker Function
In normal pacemaker function, every spike produces a response: atrial spike → P wave, or ventricular spike → QRS. In failure to capture, you see the spike but no response follows. The strip shows a spike sitting in isolation — followed by a flat line (or the underlying rhythm, if one exists) instead of the expected depolarization.
Five Criteria: Failure to Capture
- Rate: Variable (often dangerously slow)
- The effective heart rate depends on how many spikes capture and what the intrinsic escape rate is. Complete failure to capture in a pacemaker-dependent patient may result in profound bradycardia or asystole.
- Regularity: Irregular
- The pacing spikes fire regularly (on schedule), but the resulting rhythm is irregular because some spikes capture and some do not. Pauses occur after non-captured spikes.
- Pacing Spikes: Present (the pacemaker IS firing)
- This is the key distinction from failure to output. The spikes are visible on the strip — the pacemaker hardware is working and delivering energy. The problem is that the energy is not producing a myocardial response.
- Following Depolarization: Absent after some/all spikes
- The diagnostic hallmark: spikes appear without the expected P wave (atrial capture failure) or QRS (ventricular capture failure) following them.
- Pattern: Intermittent or complete
- Intermittent: some spikes capture, some do not (easier to identify — you can compare captured vs non-captured). Complete: no spikes capture at all (more dangerous — no paced output).
What Failure to Capture Looks Like on the Strip
On the strip, failure to capture shows pacing spikes that "hang in the air" — the spike appears, but the expected P wave or QRS does not follow. With intermittent failure, you see some spikes producing a response and others not — the comparison makes it obvious. With complete failure, you see regular spikes with no myocardial response, and the patient depends entirely on whatever intrinsic rhythm remains.
Failure to Capture vs Failure to Output
These are the two critical pacemaker malfunctions, and distinguishing them is straightforward: **Failure to Capture** — Spikes ARE visible, but no depolarization follows. The pacemaker fires, but the stimulus does not work. **Failure to Output** — Spikes are ABSENT when they should be present. The pacemaker is not firing at all. On the strip: see spikes without response = failure to capture. See no spikes when expected = failure to output.
Clinical Context for Monitor Technicians
Common causes of failure to capture include: lead displacement or dislodgement (the lead has moved away from the myocardium), elevated capture threshold (fibrosis at the lead tip, MI at the pacing site, electrolyte abnormalities — especially hyperkalemia), lead fracture or insulation break (energy dissipates before reaching the heart), battery depletion (inadequate energy output), and medications that increase the threshold (some antiarrhythmics).
Troubleshooting Checklist
When you see spikes without capture, work through a systematic checklist before and while you call: **1. Check the patient** — Are they symptomatic? Lightheaded, hypotensive, altered? If yes, this drives the urgency of your call. **2. Check cable connections** — Loose leads or a bad cable can distort the pacing spike and make it look like non-capture when capture is actually occurring. Tighten connections and recheck. **3. Check monitor gain** — If the gain is set too low, the capture response (the QRS after the spike) may be too small to see. Increase gain and look again. **4. Note the programmed rate vs what you are seeing** — If you have access to the programmed settings, compare. The pacing rate on the strip should match the programmed rate. **5. Report with timing** — When did non-capture start? Was it sudden or gradual? Did anything change — new medication, patient repositioning, procedure? Timing information helps the EP team narrow the cause.