Multifocal Atrial Tachycardia (MAT) — ECG Rhythm | Telemetric Pro
An irregular atrial tachycardia with at least 3 distinct P-wave morphologies at a rate exceeding 100 BPM, reflecting multiple ectopic atrial foci firing independently.
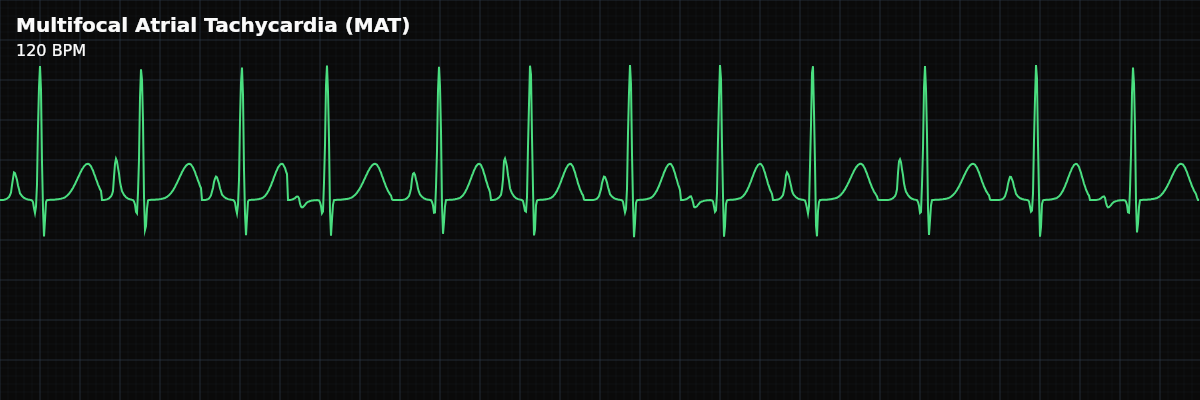
| Rate | > 100 bpm |
|---|---|
| Rhythm | Irregularly irregular |
| P Waves | At least 3 distinct morphologies |
| PR Interval | Variable |
| QRS Duration | < 0.12 s |
Multifocal Atrial Tachycardia is what happens when the atria are so irritated that multiple spots start firing on their own. Instead of one ectopic focus (as in focal atrial tachycardia), at least three different locations in the atrial tissue independently generate impulses. Each focus produces its own unique P-wave morphology, resulting in a strip that shows a different P wave nearly every beat.
For monitor technicians, MAT is important for two reasons. First, it is frequently mistaken for AFib — both are irregularly irregular, and at first glance they can look similar. Second, MAT is a red flag: it is strongly associated with severe pulmonary disease and critical illness. When you see MAT, the patient is usually very sick, and the rhythm is often a marker of the underlying disease rather than the primary problem.
What Changed from Normal Sinus Rhythm
MAT changes three things from NSR: the P-wave morphology (multiple shapes instead of one uniform shape), the regularity (irregularly irregular instead of regular), and the PR interval (variable because each focus has a different distance to the AV node). The QRS remains narrow because ventricular conduction is normal.
Five Criteria: MAT vs NSR
- Rate: >100 BPM (typically 100-150)
- Must be above 100 BPM by definition. Below 100 BPM with the same features, the rhythm is classified as Wandering Atrial Pacemaker (WAP). Rates above 150 occur in severe cases.
- Regularity: Irregularly irregular
- Both PP and RR intervals vary unpredictably. Multiple foci fire at their own independent rates, creating chaotic timing. This irregularity mimics AFib.
- P Waves: At least 3 distinct morphologies
- This is the diagnostic criterion. You must see at least 3 different P-wave shapes on the strip — each representing a different atrial focus. P waves are discrete with isoelectric baseline between them.
- PR Interval: Variable
- The PR interval changes from beat to beat because each ectopic focus has a different distance to the AV node. Shorter PR = focus closer to the AV node; longer PR = focus farther away.
- QRS Complex: Narrow (<0.12s)
- Ventricular conduction is normal. The QRS looks the same regardless of which atrial focus generated the impulse.
What MAT Looks Like on the Strip
On the strip, MAT looks like an irregular tachycardia with P waves that keep changing shape. Look at the P waves before each QRS — if you can identify at least three distinctly different P-wave morphologies (different height, width, shape, or polarity), and the baseline between P waves is flat, you are looking at MAT.
MAT vs Atrial Fibrillation
This is the most common misidentification in practice. Both are irregularly irregular, both are fast, and both can look chaotic at first glance. The distinction: **MAT** — Discrete P waves are present (at least 3 morphologies). The baseline between P waves is flat (isoelectric). Each QRS is preceded by a P wave, even though the P waves look different. **Atrial Fibrillation** — No discrete P waves. The baseline is wavy and disorganized (fibrillatory waves). QRS complexes appear randomly with no organized atrial activity preceding them.
Clinical Context for Monitor Technicians
MAT is strongly associated with severe pulmonary disease — up to 60% of cases occur in patients with COPD exacerbation. Other common associations include hypoxia, sepsis, heart failure, and electrolyte abnormalities (hypokalemia, hypomagnesemia). MAT is almost always a secondary rhythm — it reflects severe underlying illness rather than a primary cardiac problem.
Electrolyte and Medication Context
Electrolyte imbalances — particularly low potassium (hypokalemia) and low magnesium (hypomagnesemia) — are major contributors to MAT. When the clinical team repletes K+ and Mg2+, watch for gradual rhythm normalization over hours. MAT may organize into a more regular atrial rhythm (perhaps focal atrial tachycardia with a single morphology) or convert back to sinus rhythm as the electrolytes normalize. COPD medications can also trigger or worsen MAT. Albuterol nebulizers (bronchodilators given frequently during COPD exacerbations) and theophylline (a less common but still-used bronchodilator) increase atrial irritability by stimulating beta-adrenergic receptors. In a critically ill COPD patient receiving back-to-back nebulizer treatments, the medications intended to help breathing can simultaneously worsen the cardiac rhythm. If a COPD patient on continuous albuterol develops MAT, include the nebulizer schedule in your report. The clinical team may need to adjust the respiratory treatment plan to balance airway management with cardiac rhythm stability.