Junctional Escape Rhythm — ECG Rhythm | Telemetric Pro
A backup rhythm originating from the AV junction when the SA node fails, producing a regular narrow-complex bradycardia at 40-60 BPM. This is a protective mechanism against asystole.
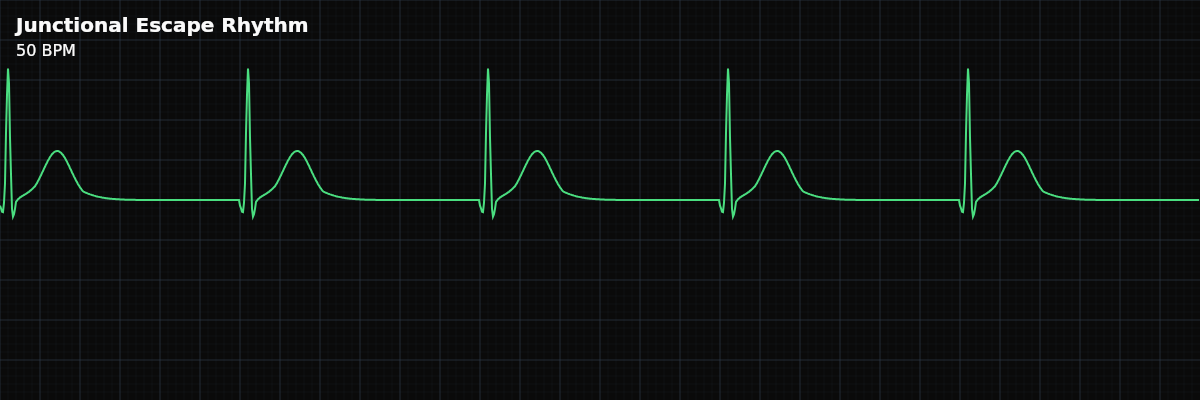
| Rate | 40–60 bpm |
|---|---|
| Rhythm | Regular |
| P Waves | Absent, retrograde, or hidden |
| PR Interval | Short (< 0.12 s) if retrograde P present |
| QRS Duration | < 0.12 s |
Junctional Escape Rhythm is the heart's first line of backup. When the SA node fails — whether from sick sinus syndrome, drug effects, or ischemia — the AV junction steps in as the pacemaker. The junction has its own automaticity (the ability to generate impulses spontaneously), but at a slower rate than the SA node: 40-60 BPM instead of 60-100.
For monitor technicians, this rhythm teaches a critical concept: escape rhythms are protective. The junctional escape exists to prevent asystole. If you see a regular narrow-complex rhythm at 40-60 BPM with no upright P waves, the SA node has likely failed, and the junction has taken over. The question is not "what is the junction doing?" — it is "why did the SA node stop?"
What Changed from Normal Sinus Rhythm
Junctional escape changes three things from NSR: the pacemaker source (AV junction instead of SA node), the rate (40-60 instead of 60-100), and the P waves (absent or retrograde instead of upright). The QRS remains narrow because the impulse still travels through the His-Purkinje system in the normal fashion.
Five Criteria: Junctional Escape vs NSR
- Rate: 40-60 BPM
- The inherent rate of the AV junction. This is the key rate range: slower than sinus (60-100), faster than ventricular escape (20-40). Below 40, consider junctional bradycardia or failing escape.
- Regularity: Regular
- The junctional pacemaker fires at a steady, consistent rate. RR intervals are equal. Unlike sinus rhythms, there is no respiratory variation.
- P Waves: Absent, retrograde, or hidden
- The impulse travels backward (retrograde) into the atria, producing inverted P waves in leads II, III, and aVF. The retrograde P may appear before the QRS (short PR), be hidden within the QRS, or follow the QRS — depending on the timing of atrial vs ventricular activation.
- PR Interval: Short (<0.12s) if P precedes QRS
- When a retrograde P wave appears before the QRS, the PR interval is very short (<0.12s) because the impulse originates near the ventricles. If P is hidden or after QRS, there is no measurable PR.
- QRS Complex: Narrow (<0.12s)
- The impulse originates at the AV junction and travels normally through the His-Purkinje system. The QRS looks identical to sinus-conducted QRS. This is the key distinction from ventricular escape (which has wide QRS).
What Junctional Escape Looks Like on the Strip
On the strip, junctional escape looks like a slow, regular rhythm with narrow QRS complexes and no upright P waves in lead II. Look carefully: retrograde P waves may appear as small inverted deflections just before the QRS, or as notches in the QRS or ST segment. At 40-60 BPM, the rhythm is distinctly slower than normal sinus.
Where Are the P Waves?
In junctional rhythms, the impulse travels in two directions simultaneously: forward (antegrade) to the ventricles and backward (retrograde) to the atria. The P-wave position on the strip depends on which direction reaches its target first: **P before QRS (short PR)** — Retrograde atrial activation occurs slightly before ventricular activation. You see an inverted P wave with a very short PR interval (<0.12s). **P hidden in QRS** — Atrial and ventricular activation occur simultaneously. The retrograde P wave is buried inside the QRS complex and cannot be seen. **P after QRS** — Ventricular activation occurs first, and the retrograde P appears after the QRS complex, often as a small inverted deflection in the ST segment.
The Junctional Rhythm Spectrum
All junctional rhythms share the same features (absent/retrograde P waves, narrow QRS) — they differ only by rate: **Junctional Escape** — 40-60 BPM. The junction's inherent rate. Occurs when the SA node fails (protective). **Accelerated Junctional** — 60-100 BPM. The junction fires faster than normal due to enhanced automaticity. The junction competes with or usurps the SA node. **Junctional Tachycardia** — >100 BPM. Abnormally enhanced junctional automaticity. Usually indicates underlying pathology (digoxin toxicity, post-cardiac surgery, ischemia).
Clinical Context for Monitor Technicians
Junctional escape occurs when the SA node fails or its impulses are blocked. Common causes include sick sinus syndrome, medications that suppress the SA node (beta-blockers, calcium channel blockers, digoxin), inferior MI affecting the SA node artery, and high vagal tone (athletes, during sleep). In athletes and young patients, a junctional escape during sleep may be a benign finding.
When to Escalate
**Notify promptly:** - New junctional escape rhythm (SA node failure is implied — the team needs to investigate why) - Patient is symptomatic — dizziness, syncope, hypotension, altered consciousness - Rate drops below 40 BPM (the junction may also be failing) - Junctional escape follows a period of sinus arrest or complete heart block **Document and monitor:** - Known junctional escape in a stable, asymptomatic patient - Junctional rhythm during sleep in a young/athletic patient (likely vagal)