Junctional Bradycardia — ECG Rhythm | Telemetric Pro
A severely slow junctional rhythm below 40 BPM. It shares junctional P-wave behavior with narrow QRS but carries higher urgency because ventricular rate may be insufficient for perfusion.
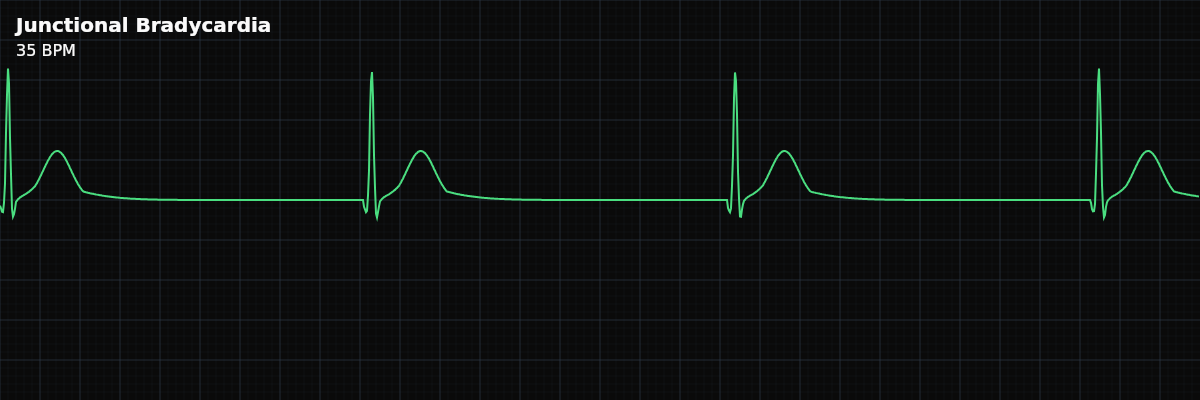
| Rate | < 40 bpm |
|---|---|
| Rhythm | Usually regular |
| P Waves | Absent, retrograde, or hidden |
| PR Interval | Short (< 0.12 s) if retrograde P present |
| QRS Duration | < 0.12 s |
Junctional bradycardia sits below the AV junction's inherent 40-60 BPM rate. It keeps the same junctional origin features as junctional escape, but the slower ventricular output raises concern for poor perfusion and deterioration.
Five Criteria Snapshot
- Rate: <40 BPM
- This is slower than standard junctional escape and should be treated as a high-urgency finding.
- Regularity: Usually regular
- RR intervals are often consistent unless superimposed ectopy or progression occurs.
- P waves: Absent or retrograde
- P waves may be retrograde (traveling backward, from the AV junction upward toward the atria) — appearing inverted before QRS, hidden in QRS, or after QRS.
- PR interval: Short if present
- If an inverted P precedes QRS, PR is typically <0.12s.
- QRS: Narrow
- Narrow QRS supports junctional origin rather than ventricular-origin brady rhythms.
High-Yield Differentials
Monitor-Tech Escalation Focus
Treat junctional bradycardia as high urgency from the monitoring station: report rate and morphology immediately, time-stamp onset, print strips, and watch for progression below 30 BPM, pauses, or transition to ventricular escape/asystole.
Medication Causes
Several common cardiac medications can slow the AV junction enough to push a junctional rhythm into bradycardia territory. Beta-blockers (metoprolol, atenolol) reduce automaticity across all pacemaker sites, including the AV junction. Calcium channel blockers (diltiazem, verapamil) slow conduction through the AV node directly. Digoxin enhances vagal tone on the AV junction and at higher levels can suppress junctional automaticity altogether. Any of these — alone or in combination — can take a stable junctional escape at 50 BPM and push it down to 35. If a patient on one of these medications develops junctional bradycardia, include the medication name and the time of the last dose in your report. That timing helps the clinical team decide whether to hold the next dose or intervene.
What Happens When Treatment Is Given
Atropine is typically the first medication used for symptomatic junctional bradycardia. It blocks vagal input to the AV junction, which can increase the junctional rate — often within one to two minutes of administration. On the monitor, you will see the heart rate climb and the rhythm may remain junctional or transition back to sinus. If atropine does not increase the rate, the clinical team may move to transcutaneous pacing. When pacing is initiated, you will see tall, wide pacing spikes on the monitor — vertical deflections much larger than the native QRS. Your job is to confirm electrical capture: each pacing spike should be followed by a wide QRS complex. Report any spikes without capture immediately.
Progression Risk
Junctional bradycardia can deteriorate in a predictable downward sequence: junctional bradycardia → idioventricular rhythm (IVR) → asystole. Each step represents the pacemaker site falling lower in the conduction system. Junctional bradycardia originates at the AV junction and produces a narrow QRS. When the junction fails, ventricular cells take over as the last-resort pacemaker — IVR — producing a wide, slow QRS at 20-40 BPM. If that ventricular pacemaker also fails, the result is asystole. The key morphology change to watch for: narrow QRS suddenly replaced by wide QRS at the same or slower rate. That shift means ventricular escape has taken over and the patient has lost their junctional pacemaker.
Symptomatic Threshold
Junctional rates below 40-50 BPM are frequently symptomatic because the cardiac output drops below what the body needs. From the monitoring station, you may not be at the bedside, but you can still identify signs of poor perfusion on your displays: blood pressure trending downward on the vitals column, oxygen saturation drifting from the mid-90s into the low 90s or 80s, or rhythm-correlated alarms firing on multiple parameters at once. The patient may activate the call light reporting dizziness, lightheadedness, or "feeling faint." Any of these combined with a junctional rate in the 30s should prompt immediate escalation — do not wait for the next scheduled vitals check.