Biventricular Paced Rhythm (CRT) — ECG Rhythm | Telemetric Pro
Cardiac Resynchronization Therapy paces both ventricles simultaneously to restore synchronized contraction. The QRS has a characteristic notched or M-shaped pattern that is narrower than standard RV-only pacing.
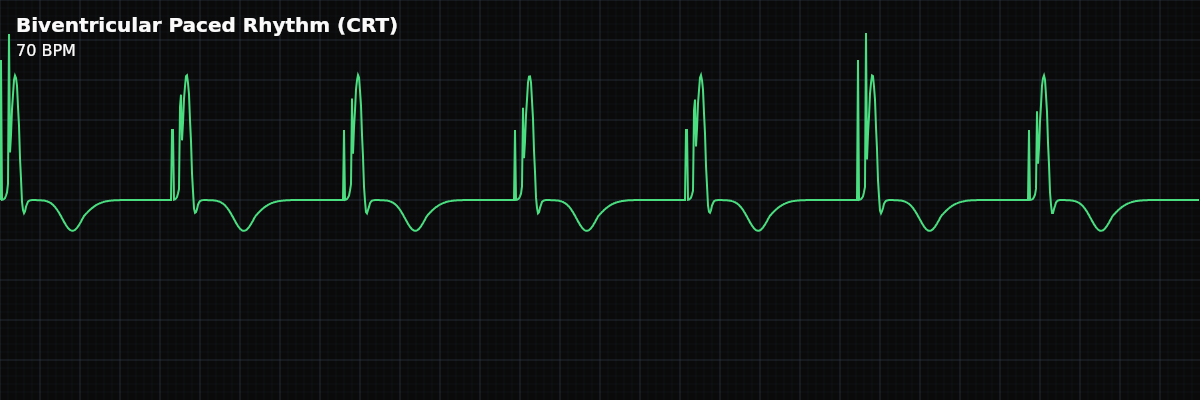
| Rate | 60–130 bpm (programmed) |
|---|---|
| Rhythm | Regular |
| P Waves | Pacing spike or native (depends on mode) |
| PR Interval | Programmed AV delay |
| QRS Duration | May be narrower than native LBBB (resynchronized) |
Biventricular pacing — Cardiac Resynchronization Therapy (CRT) — is a specialized pacing mode designed for heart failure patients with ventricular dyssynchrony (where the left and right ventricles contract out of sync). By pacing both ventricles simultaneously, CRT restores coordinated contraction and improves cardiac output. The QRS morphology on the monitor is distinctive: it is wide (because both ventricles are paced), but narrower than standard RV-only pacing, and often has a characteristic notched or M-shaped pattern.
For monitor technicians, CRT is important because these patients are often critically dependent on biventricular pacing. If the left ventricular lead loses capture or the device reverts to single-site RV pacing, the patient can decompensate rapidly. Recognizing the change in QRS morphology — from the characteristic CRT pattern to wider single-site pacing — is a key monitoring skill.
What Changed from Normal Sinus Rhythm
CRT changes the QRS morphology and width compared to NSR. The QRS is wide (because both ventricles are paced from electrodes, not through the normal conduction system) but has a unique morphology that differs from both native LBBB and standard RV pacing. The notched or M-shaped QRS reflects the two wavefronts colliding as depolarization spreads from both pacing sites simultaneously.
Five Criteria: CRT vs NSR
- Rate: Programmed (typically 60-130 BPM)
- Usually has rate-responsive features enabled. Most CRT devices also pace the atrium (CRT-P = pacemaker only, CRT-D = pacemaker plus defibrillator), providing AV synchrony.
- Regularity: Regular
- Consistent pacing intervals. The rhythm is regular unless the patient has breakthrough atrial fibrillation (which can reduce biventricular pacing percentage).
- P Waves: Paced or native (depending on device mode)
- Most CRT devices also pace the atrium — you may see an atrial spike before the P wave. Some devices sense native P waves and trigger biventricular pacing (like DDD mode).
- PR Interval: Programmed AV delay
- The interval between the atrial event (paced or sensed) and the biventricular stimulus is a programmed AV delay optimized for the patient.
- QRS Complex: Wide but characteristic (120-160ms, notched)
- Narrower than standard RV pacing (~120-160ms vs ~180ms). Notched or M-shaped pattern. V1 may show positive or biphasic deflection (unlike pure LBBB of RV pacing).
What CRT Looks Like on the Strip
On the monitor, CRT looks like a paced rhythm with a QRS that is wider than normal but narrower than typical RV pacing. The key recognition feature is the notched or M-shaped QRS morphology — the result of two depolarization wavefronts meeting from the RV and LV pacing sites. Compare to the patient's baseline CRT morphology: any widening suggests loss of one lead's capture.
Recognizing Loss of Biventricular Capture
Loss of biventricular capture is one of the most important things to watch for in CRT patients: **Normal CRT capture** — Characteristic notched QRS, narrower width (~120-160ms), unique morphology. **Loss of LV lead capture** — QRS widens, morphology changes to pure LBBB pattern (like standard RV pacing). The QRS looks like VVI pacing because only the RV lead is capturing. **Loss of RV lead capture** — QRS morphology changes but may be less obviously different. Compare to baseline.
Clinical Context for Monitor Technicians
CRT is used in heart failure patients with ventricular dyssynchrony (typically LBBB with QRS > 150ms and reduced ejection fraction — the percentage of blood the heart pumps out with each beat). The goal is to restore synchronized ventricular contraction, which improves cardiac output and symptoms. Maintaining a high biventricular pacing percentage (> 95%) is critical for therapeutic benefit — anything that reduces BiV pacing (atrial fibrillation with rapid response, frequent PVCs) can diminish the benefit.
When to Escalate
**Notify promptly:** - QRS morphology changes (possible loss of BiV capture) - QRS widens to standard RV pacing morphology (loss of LV lead capture) - New atrial fibrillation with rapid response (reduces BiV pacing percentage) - Patient becomes symptomatic — worsening dyspnea, fatigue, fluid retention - Frequent PVCs reducing BiV pacing percentage **Document and monitor:** - Stable BiV pacing with consistent QRS morphology matching baseline - Rate-responsive behavior during patient activity
What Happens When...
**Patient exercises** — Most CRT devices have rate-responsive features enabled. The pacing rate increases with activity, and that is normal. You will see a faster biventricular paced rhythm with the same characteristic notched QRS morphology. The rate rise is programmed behavior, not a malfunction. **New AFib develops** — This is the most critical scenario for CRT patients. Atrial fibrillation reduces biventricular pacing percentage because the device cannot track P waves during AFib. The ventricles may be activated by conducted AFib impulses instead of by the biventricular pacemaker. If BiV pacing drops below approximately 90% in a CRT patient, the therapeutic benefit is lost. Report new atrial fibrillation in these patients promptly — it directly undermines the reason the device was implanted. **Threshold testing** — During electrophysiology device interrogation, the clinical team may temporarily reduce pacing output to test capture thresholds for each ventricular lead independently. Brief periods of capture loss or changes in QRS morphology are expected during this procedure. **Battery near end-of-life** — As the battery depletes, the device may switch modes automatically (for example, DDD to VVI). You may notice a change in the pacing pattern, and the rate may decrease. In CRT devices, mode switching can mean loss of biventricular pacing — the device may revert to single-chamber RV pacing. Watch for QRS morphology changes that suggest loss of BiV capture. **Electromagnetic interference (EMI)** — Strong electromagnetic fields can cause noise on the monitor or inappropriate pacemaker inhibition. You may see artifact or pauses in pacing. If you suspect EMI, verify the patient's clinical status and look for nearby equipment sources.