Accelerated Idioventricular Rhythm (AIVR) — ECG Rhythm | Telemetric Pro
A wide-complex ventricular rhythm at 50-100 BPM — faster than ventricular escape but slower than VT. Usually transient, benign, and classically associated with myocardial reperfusion.
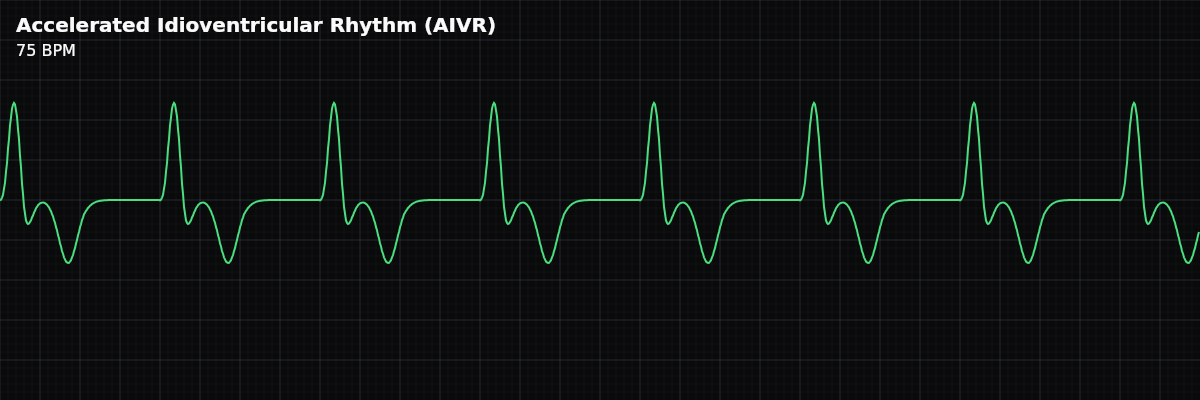
| Rate | 50–100 bpm |
|---|---|
| Rhythm | Regular |
| P Waves | Absent |
| PR Interval | Not applicable |
| QRS Duration | > 0.12 s (wide) |
AIVR occupies a unique position in the ventricular rhythm spectrum: it is a wide-complex rhythm that is usually benign. The ventricular pacemaker cells are firing faster than their inherent escape rate (20-40 BPM) but slower than true ventricular tachycardia (>100 BPM). This "accelerated" but not "tachycardic" rate is what gives AIVR its distinctive clinical profile.
For monitor technicians, AIVR is important because it looks scary — wide QRS complexes always raise the alarm for VT. But AIVR at 50-100 BPM in the right clinical context (post-PCI, post-thrombolysis, reperfusion) is actually a reassuring sign. The key skill is distinguishing it from VT by the rate and clinical context.
What Changed from Normal Sinus Rhythm
AIVR changes the pacemaker source (ventricles instead of SA node) and the QRS (wide instead of narrow). Unlike IVR (which is an escape rhythm indicating failure of higher pacemakers), AIVR occurs because the ventricular pacemaker cells are enhanced — firing faster than normal, often competing with the sinus rate.
Five Criteria: AIVR vs NSR
- Rate: 50-100 BPM
- Falls in the normal heart rate range, which is why it is usually hemodynamically tolerated. Faster than IVR escape (20-40) but distinctly slower than VT (>100).
- Regularity: Regular (with gradual onset/offset)
- The rhythm is usually regular. It characteristically shows a gradual warm-up at onset and cool-down at termination — the rate accelerates over several beats, then decelerates before stopping.
- P Waves: Dissociated or absent
- AV dissociation is the norm — the SA node fires the atria and the ventricular focus fires the ventricles independently. P waves may be visible marching at a different rate than the QRS complexes.
- PR Interval: Not applicable
- The atria and ventricles are electrically independent. P waves bear no consistent timing relationship to QRS complexes.
- QRS Complex: Wide (>0.12s)
- Wide because the impulse originates in the ventricular myocardium. The morphology is monomorphic (each wide QRS looks the same) — unlike polymorphic VT where the QRS changes shape.
What AIVR Looks Like on the Strip
On the strip, AIVR looks like a wide-complex rhythm at a rate that feels "too slow for VT." The QRS complexes are wide and monomorphic (all look the same). You may see the rhythm gradually emerge from normal sinus as the ventricular rate exceeds the sinus rate, and gradually recede back to sinus as the ventricular rate slows. Fusion beats (intermediate-width QRS) at the transitions are a hallmark.
AIVR vs Ventricular Tachycardia
Both are wide-complex ventricular rhythms, but the rate and clinical significance are very different: **AIVR (50-100 BPM)** — Usually benign and self-limiting. Gradual onset/offset. Hemodynamically stable. Often a reperfusion sign. Do NOT suppress. **VT (>100 BPM)** — Potentially life-threatening. Abrupt onset. May be hemodynamically unstable. Requires treatment. The cutoff is approximately 100 BPM — above that rate, treat as VT until proven otherwise.
Clinical Context for Monitor Technicians
AIVR is most commonly seen during myocardial reperfusion — after successful PCI or thrombolysis for acute MI. In this context, it is a positive sign that the blocked coronary artery has been reopened. Other causes include digoxin toxicity, myocarditis, electrolyte abnormalities, and post-cardiac arrest as ventricular automaticity recovers.
When to Escalate
**Notify promptly:** - New wide-complex rhythm (even if you suspect AIVR, the team needs to confirm) - Rate approaches or exceeds 100 BPM (crosses into VT territory) - Patient becomes symptomatic — hypotension, dizziness, chest pain - AIVR does not resolve after a reasonable observation period **Document and monitor:** - AIVR at 50-100 BPM in a stable post-PCI or post-thrombolysis patient - Known AIVR that is transient and self-resolving
Putting It Together
AIVR is a wide-complex ventricular rhythm at 50-100 BPM — faster than ventricular escape but slower than VT. It is usually benign, transient, and associated with myocardial reperfusion. Do NOT suppress it with antiarrhythmics. Distinguish from VT by rate (<100 vs >100). Fusion and capture beats at the transitions between AIVR and sinus rhythm are supporting diagnostic features.