Third Degree AV Block (Ventricular Escape) — ECG Rhythm | Telemetric Pro
Complete heart block with a wide-QRS ventricular escape rhythm. The block is below the bundle bifurcation (infranodal), so the escape pacemaker originates in the ventricular conduction tissue. More urgent than junctional-escape complete heart block — the escape is unreliable and is a Class I indication for permanent pacing.
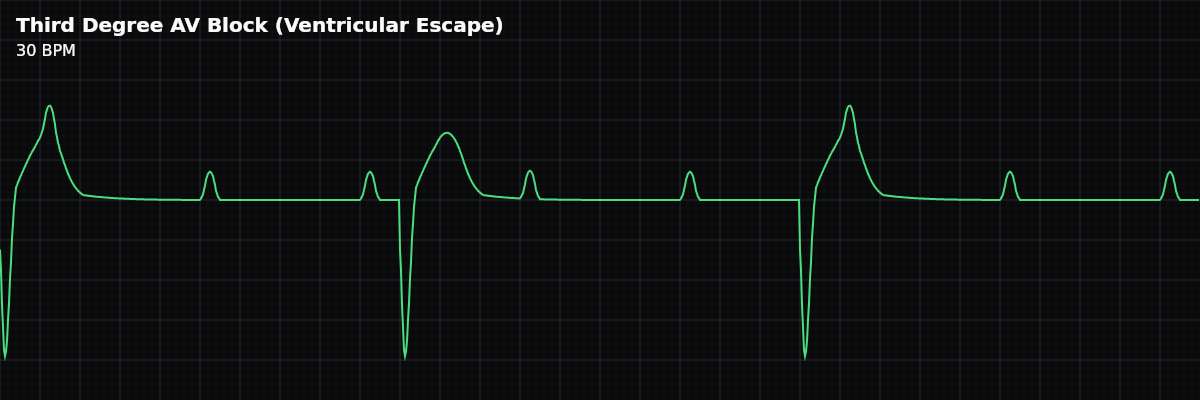
| Rate | Ventricular 25–40 bpm; atrial 60–100 bpm (clear gap) |
|---|---|
| Rhythm | Regular (P and QRS each regular, independent, ~3:1 ratio) |
| P Waves | Present, march clearly through TP segments at sinus rate |
| PR Interval | Variable (no relationship to QRS) |
| QRS Duration | Wide (≥120 ms), bizarre — ventricular/fascicular escape |
Third Degree AV Block with Ventricular Escape is the more severe form of complete heart block. Unlike junctional-escape CHB (where the AV node fails but the junction takes over with a narrow, reasonably stable rhythm), here the block is *below* the bundle bifurcation. The His-Purkinje system has failed and the only thing keeping the patient alive is a slow, wide, bizarre escape from ventricular tissue itself.
For monitor technicians, this is the textbook "complete heart block strip" you remember from training: P waves marching clearly at sinus rate while wide bizarre QRS complexes occur at 25-40 bpm with no relationship between them. The visual is unmistakable because the rate gap is so large (often 3:1 P-to-QRS) and the QRS complexes are clearly abnormal in shape.
How It Differs from Junctional-Escape CHB
Five Criteria: Ventricular-Escape CHB
- Rate: Slow ventricular (25-40), normal-to-fast atrial (60-100)
- The atrial rate is normal sinus or mildly elevated (compensatory response to low cardiac output). The ventricular rate is the escape: 20-40 bpm. The gap between atrial and ventricular rates is large — often a clean 3:1 ratio.
- Regularity: Both rhythms regular, independent
- P-P intervals are regular (atrial rhythm runs on its own). R-R intervals are also regular (escape rhythm runs on its own). They are at clearly different rates with no relationship.
- P Waves: Marching clearly through TP segments
- Sinus P waves are visible between QRS complexes — usually 2-3 P waves per cycle. Because the ratio is approximately 3:1 and the rates are clearly different, the marching pattern is visually obvious. This is the textbook "P waves marching through" appearance.
- PR Interval: Variable, meaningless
- There is no PR interval to measure because there is no conduction between P and QRS. P waves land in random positions relative to the QRS — sometimes in front, sometimes buried, sometimes after.
- QRS: Wide (≥120 ms), bizarre, ventricular morphology
- The wide bizarre QRS is the signature of ventricular escape. It looks like a PVC or VT beat, but slow. T wave is usually discordant (opposite direction from the main QRS deflection).
What Ventricular-Escape CHB Looks Like on the Strip
The visual is unmistakable: wide bizarre QRS complexes spaced far apart, with clearly visible upright P waves marching between them in the long TP segments. Use calipers — drop them on any two consecutive P waves and walk them across the strip. The P-P interval should stay constant (sinus regular). Then drop calipers on the QRS complexes — the R-R interval is also constant, just at a slower rate. Two regular rhythms running independently at different speeds.
Why the Rate Gap Matters Clinically
In junctional-escape CHB, the rates can be relatively close (atrial 75, ventricular 50 — a 25 bpm gap). In ventricular-escape CHB, the gap is much wider (atrial 90, ventricular 30 — a 60 bpm gap). The wider the gap, the more obvious the dissociation visually, and the more profound the conduction failure clinically. A wide gap also tells you that the escape pacemaker is firing from a low, unreliable focus — the lower the escape, the worse the prognosis.
Clinical Context for Monitor Technicians
Ventricular-escape CHB is most commonly seen in: anterior MI (LAD distribution — the LAD supplies the bundle branches, so anterior infarction causes infranodal block), Lev disease (idiopathic fibrosis of the cardiac skeleton extending into the conduction tissue, typically in older patients), Lenègre disease (primary degenerative disease of the conduction system), severe hyperkalemia, drug toxicity (Class I antiarrhythmics, tricyclics), and post-cardiac surgery (especially valve replacement).
When to Escalate
**Notify immediately, every time.** Wide-QRS complete heart block is never a "watch and wait" rhythm. **Notify with even higher urgency if:** - The escape rate is dropping below 25 bpm or becoming irregular (escape failure imminent) - The patient is symptomatic — syncope, altered consciousness, hypotension, cool/clammy skin - The escape rhythm has long pauses between beats (precursor to asystole) - You see new ventricular-escape CHB in an acute MI patient (especially anterior MI)